Abstract
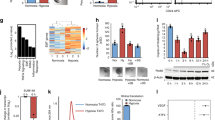
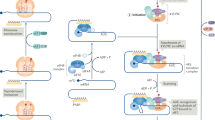
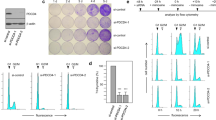
Malignant transformation, invasion and angiogenesis rely on the coordinated reprogramming of gene expression in the cells from which the tumor originated. Although deregulated gene expression has been extensively studied at genomic and epigenetic scales, the contribution of the regulation of mRNA-specific translation to this reprogramming is not well understood. Here we show that cytoplasmic polyadenylation element binding protein 4 (CPEB4), an RNA binding protein that mediates meiotic mRNA cytoplasmic polyadenylation and translation, is overexpressed in pancreatic ductal adenocarcinomas and glioblastomas, where it supports tumor growth, vascularization and invasion. We also show that, in pancreatic tumors, the pro-oncogenic functions of CPEB4 originate in the translational activation of mRNAs that are silenced in normal tissue, including the mRNA of tissue plasminogen activator, a key contributor to pancreatic ductal adenocarcinoma malignancy. Taken together, our results document a key role for post-transcriptional gene regulation in tumor development and describe a detailed mechanism for gene expression reprogramming underlying malignant tumor progression.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Hanahan, D. & Weinberg, R.A. The hallmarks of cancer. Cell 100, 57–70 (2000).
Mayr, C., Hemann, M.T. & Bartel, D.P. Disrupting the pairing between let-7 and Hmga2 enhances oncogenic transformation. Science 315, 1576–1579 (2007).
Lee, Y.S. & Dutta, A. The tumor suppressor microRNA let-7 represses the HMGA2 oncogene. Genes Dev. 21, 1025–1030 (2007).
Sonenberg, N. & Hinnebusch, A.G. Regulation of translation initiation in eukaryotes: mechanisms and biological targets. Cell 136, 731–745 (2009).
Silvera, D., Formenti, S.C. & Schneider, R.J. Translational control in cancer. Nat. Rev. Cancer 10, 254–266 (2010).
Piqué, M., Lopez, J.M., Foissac, S., Guigo, R. & Mendez, R. A combinatorial code for CPE-mediated translational control. Cell 132, 434–448 (2008).
Belloc, E. & Mendez, R. A deadenylation negative feedback mechanism governs meiotic metaphase arrest. Nature 452, 1017–1021 (2008).
Eliscovich, C., Peset, I., Vernos, I. & Mendez, R. Spindle-localized CPE-mediated translation controls meiotic chromosome segregation. Nat. Cell Biol. 10, 858–865 (2008).
Novoa, I., Gallego, J., Ferreira, P.G. & Mendez, R. Mitotic cell-cycle progression is regulated by CPEB1- and CPEB4-dependent translational control. Nat. Cell Biol. 12, 447–456 (2010).
Mendez, R. & Richter, J.D. Translational control by CPEB: a means to the end. Nat. Rev. Mol. Cell Biol. 2, 521–529 (2001).
Groppo, R. & Richter, J.D. Translational control from head to tail. Curr. Opin. Cell Biol. 21, 444–451 (2009).
Igea, A. & Mendez, R. Meiosis requires a translational positive loop where CPEB1 ensues its replacement by CPEB4. EMBO J. 29, 2182–2193 (2010).
Huang, Y.S., Kan, M.C., Lin, C.L. & Richter, J.D. CPEB3 and CPEB4 in neurons: analysis of RNA-binding specificity and translational control of AMPA receptor GluR2 mRNA. EMBO J. 25, 4865–4876 (2006).
Groisman, I. et al. Control of cellular senescence by CPEB. Genes Dev. 20, 2701–2712 (2006).
Richter, J.D. CPEB: a life in translation. Trends Biochem. Sci. 32, 279–285 (2007).
Burns, D.M. & Richter, J.D. CPEB regulation of human cellular senescence, energy metabolism, and p53 mRNA translation. Genes Dev. 22, 3449–3460 (2008).
Jones, S. et al. Core signaling pathways in human pancreatic cancers revealed by global genomic analyses. Science 321, 1801–1806 (2008).
Parsons, D.W. et al. An integrated genomic analysis of human glioblastoma multiforme. Science 321, 1807–1812 (2008).
Iacobuzio-Donahue, C.A. et al. DPC4 gene status of the primary carcinoma correlates with patterns of failure in patients with pancreatic cancer. J. Clin. Oncol. 27, 1806–1813 (2009).
van Riggelen, J., Yetil, A. & Felsher, D.W. MYC as a regulator of ribosome biogenesis and protein synthesis. Nat. Rev. Cancer 10, 301–309 (2010).
Paciucci, R. et al. Isolation of tissue-type plasminogen activator, cathepsin H, and non- specific cross-reacting antigen from SK-PC-1 pancreas cancer cells using subtractive hybridization. FEBS Lett. 385, 72–76 (1996).
Paciucci, R., Tora, M., Diaz, V.M. & Real, F.X. The plasminogen activator system in pancreas cancer: role of t-PA in the invasive potential in vitro. Oncogene 16, 625–633 (1998).
Díaz, V.M., Planaguma, J., Thomson, T.M., Reventos, J. & Paciucci, R. Tissue plasminogen activator is required for the growth, invasion, and angiogenesis of pancreatic tumor cells. Gastroenterology 122, 806–819 (2002).
Ryu, B. et al. Relationships and differentially expressed genes among pancreatic cancers examined by large-scale serial analysis of gene expression. Cancer Res. 62, 819–826 (2002).
Iacobuzio-Donahue, C.A. et al. Highly expressed genes in pancreatic ductal adenocarcinomas: a comprehensive characterization and comparison of the transcription profiles obtained from three major technologies. Cancer Res. 63, 8614–8622 (2003).
Aguilar, S. et al. Tissue plasminogen activator in murine exocrine pancreas cancer: selective expression in ductal tumors and contribution to cancer progression. Am. J. Pathol. 165, 1129–1139 (2004).
Missiaglia, E. et al. Analysis of gene expression in cancer cell lines identifies candidate markers for pancreatic tumorigenesis and metastasis. Int. J. Cancer 112, 100–112 (2004).
Huarte, J., Belin, D., Vassalli, A., Strickland, S. & Vassalli, J.D. Meiotic maturation of mouse oocytes triggers the translation and polyadenylation of dormant tissue-type plasminogen activator mRNA. Genes Dev. 1, 1201–1211 (1987).
Shin, C.Y., Kundel, M. & Wells, D.G. Rapid, activity-induced increase in tissue plasminogen activator is mediated by metabotropic glutamate receptor-dependent mRNA translation. J. Neurosci. 24, 9425–9433 (2004).
Gardina, P.J. et al. Alternative splicing and differential gene expression in colon cancer detected by a whole genome exon array. BMC Genomics 7, 325 (2006).
Karni, R. et al. The gene encoding the splicing factor SF2/ASF is a proto-oncogene. Nat. Struct. Mol. Biol. 14, 185–193 (2007).
Srebrow, A. & Kornblihtt, A.R. The connection between splicing and cancer. J. Cell Sci. 119, 2635–2641 (2006).
Karni, R., Hippo, Y., Lowe, S.W. & Krainer, A.R. The splicing-factor oncoprotein SF2/ASF activates mTORC1. Proc. Natl. Acad. Sci. USA 105, 15323–15327 (2008).
Cooper, C. et al. Increasing the relative expression of endogenous non-coding steroid receptor RNA activator (SRA) in human breast cancer cells using modified oligonucleotides. Nucleic Acids Res. 37, 4518–4531 (2009).
Pio, R. & Montuenga, L.M. Alternative splicing in lung cancer. J. Thorac. Oncol. 4, 674–678 (2009).
Mayr, C. & Bartel, D.P. Widespread shortening of 3′ UTRs by alternative cleavage and polyadenylation activates oncogenes in cancer cells. Cell 138, 673–684 (2009).
Ji, Z. & Tian, B. Reprogramming of 3′ untranslated regions of mRNAs by alternative polyadenylation in generation of pluripotent stem cells from different cell types. PLoS ONE 4, e8419 (2009).
Blasi, F. & Sidenius, N. The urokinase receptor: focused cell surface proteolysis, cell adhesion and signaling. FEBS Lett. 584, 1923–1930 (2010).
Ossowski, L. Plasminogen activator dependent pathways in the dissemination of human tumor cells in the chick embryo. Cell 52, 321–328 (1988).
Aguirre-Ghiso, J.A., Liu, D., Mignatti, A., Kovalski, K. & Ossowski, L. Urokinase receptor and fibronectin regulate the ERK(MAPK) to p38(MAPK) activity ratios that determine carcinoma cell proliferation or dormancy in vivo. Mol. Biol. Cell 12, 863–879 (2001).
Smith, H.W. & Marshall, C.J. Regulation of cell signalling by uPAR. Nat. Rev. Mol. Cell Biol. 11, 23–36 (2010).
Ulisse, S., Baldini, E., Sorrenti, S. & D'Armiento, M. The urokinase plasminogen activator system: a target for anti-cancer therapy. Curr. Cancer Drug Targets 9, 32–71 (2009).
McMahon, B. & Kwaan, H.C. The plasminogen activator system and cancer. Pathophysiol. Haemost. Thromb. 36, 184–194 (2008).
Huarte, J., Belin, D. & Vassalli, J.D. Plasminogen activator in mouse and rat oocytes: induction during meiotic maturation. Cell 43, 551–558 (1985).
Huarte, J. et al. Transient translational silencing by reversible mRNA deadenylation. Cell 69, 1021–1030 (1992).
Gandin, V. et al. Eukaryotic initiation factor 6 is rate-limiting in translation, growth and transformation. Nature 455, 684–688 (2008).
Ruggero, D. et al. The translation factor eIF-4E promotes tumor formation and cooperates with c-Myc in lymphomagenesis. Nat. Med. 10, 484–486 (2004).
Livingstone, M., Atas, E., Meller, A. & Sonenberg, N. Mechanisms governing the control of mRNA translation. Phys. Biol. 7, 021001 (2010).
Janic, A., Mendizabal, L., Llamazares, S., Rossell, D. & Gonzalez, C. Ectopic expression of germline genes drives malignant brain tumor growth in Drosophila. Science 330, 1824–1827 (2010).
Gaspar, C. et al. Cross-species comparison of human and mouse intestinal polyps reveals conserved mechanisms in adenomatous polyposis coli (APC)-driven tumorigenesis. Am. J. Pathol. 172, 1363–1380 (2008).
Sääf, A.M. et al. Parallels between global transcriptional programs of polarizing Caco-2 intestinal epithelial cells in vitro and gene expression programs in normal colon and colon cancer. Mol. Biol. Cell 18, 4245–4260 (2007).
Read, T.A. et al. Identification of CD15 as a marker for tumor-propagating cells in a mouse model of medulloblastoma. Cancer Cell 15, 135–147 (2009).
Chen, H.Y. et al. A five-gene signature and clinical outcome in non-small-cell lung cancer. N. Engl. J. Med. 356, 11–20 (2007).
Israel, A., Sharan, R., Ruppin, E. & Galun, E. Increased microRNA activity in human cancers. PLoS ONE 4, e6045 (2009).
Hansen, C.N. et al. Expression of CPEB, GAPDH and U6snRNA in cervical and ovarian tissue during cancer development. APMIS 117, 53–59 (2009).
Roda, O. et al. Galectin-1 is a novel functional receptor for tissue plasminogen activator in pancreatic cancer. Gastroenterology 136, 1379–1390 (2009).
Rizzino, A. Behavior of transforming growth factors in serum-free media: an improved assay for transforming growth factors. In Vitro 20, 815–822 (1984).
Huch, M. et al. Urokinase-type plasminogen activator receptor transcriptionally controlled adenoviruses eradicate pancreatic tumors and liver metastasis in mouse models. Neoplasia 11, 518–528 (2009).
Acknowledgements
The authors acknowledge F. Gebauer, S. Aznar-Benitah, A. García de Herreros and J. Valcárcel for critical comments on the manuscript and for other valuable contributions. We also thank S. Hahn (Department of Molecular GI-Oncology, University of Bochum, Germany) and M. Buchholz (Department of Gastroenterology, Endocrinology and Metabolism, Philipps-University of Marburg, Marburg, Germany) for providing normal pancreas RNA, O. Casanovas (Translational Research Laboratory, Catalan Institute of Oncology (ICO)–Bellvitge Biomedical Research Institute (IDIBELL), L'Hospitalet de Llobregat, Spain) for his help with the T98G nude mice injections, J.R. González-Vallinas (Computational Genomics Group, Universitat Pompeu Fabra, Parc de Recerca Biomèdica de Barcelona (PRBB)) for assistance with Gene Ontology tools and E. Castillo from the Ultrasequencing Unit (Centre for Genomic Regulation, PRBB), S. Mojal from the Statistics Unit (IMIM, PRBB) and T. Lobato from the Histopathological Unit (IMIM, PRBB) for technical assistance. This work was funded by the research grants Instituto de Salud Carlos–Fondos Europeos de Desarrollo Regional (FEDER) (PI080421) from the Ministerio de Ciencia e Innovación (MICINN) and grants from Fundació La MaratóTV3 (051110), the American Institute for Cancer Research (AICR) (11-0086) and Generalitat de Catalunya (2009SGR1409) to P.N.; grants BFU2008-02373 and Consolider RNAREG CSD2009-00080 from the MICINN and grants from Fundació La MaratóTV3 (051110), AICR (11-0086) and Generalitat de Catalunya (2009SGR1436) to R.M.; grant SAF2007-60860 and Consolider ONCOBIO from the MICINN and a grant from the VI EU Framework Programme MolDiag-PaCa project to F.X.R.; grants Consolider RNAREG CSD2009-00080 and BIO2008-01091 from the MICINN to E.E.; and grants from the Instituto de Salud Carlos III FEDER (RD09/0076/00036) and the Xarxa de Bancs de tumors sponsored by the Pla Director d'Oncologia de Catalunya to the MARBiobanc. P.N. is supported by the Instituto de Salud Carlos III and the Departament de Sanitat de la Generalitat de Catalunya. D.P. holds a Juan de la Cierva grant from the MICINN. N.M.-B. holds a grant from the Fundación Ramón Areces. C.E. was supported by a fellowship from the DURSI (Generalitat de Catalunya) and Fons Social Europeu (ESF).
Author information
Authors and Affiliations
Contributions
E.O.-Z. performed the experiments shown in Figures 1,2,3,4,5,6 and in Supplementary Figures 1, 3, 4 and 6–10, prepared the figures for the manuscript (except Fig. 5b) and contributed to the experimental design of the study and the preparation of the manuscript. D.P. generated the majority of the plasmids used in the study, designed the primers for the RIP validation experiments, helped with the frog surgery, injection of the oocytes, reporter analyses and in vivo experiments and prepared Figures 5b, 6d and 6f and Supplementary Figure 2. N.M.-B. established the RWP-1 LUC cell line, helped with the in vivo experiments, performed immunohistochemistry analyses of the Capan-1 xenografts and performed all the statistical analyses. D.P. and N.M.-B. prepared Figure 3 and Supplementary Figure 5 and made useful contributions to the experimental design and the interpretation of the data. G.F.-M. generated Capan-1 shCtrl and shCPEB4 cells and contributed to the interpretation of the data. M.I. supplied all the human pancreatic samples used in the study and helped with the histopathological analyses of all the immunohistochemistries performed in samples from both mice and humans. F.A. supplied human glioblastoma samples and helped with the histopathological and immunohistochemistries analyses in tumors from both mice and humans. M.M. helped with the in vivo experiments. C.E. generated the data shown at the bottom of Figure 6b. E.E. performed the analysis of the data generated in the Illumina Solexa sequencing, performed the motif analysis of the 3′ UTR sequences shown in Figure 5a, generated the data shown in Supplementary Figures 6 and 7 and contributed to the preparation of the manuscript. F.X.R. contributed to the study design, data analysis and manuscript preparation. P.N. and R.M. directed the study and wrote the manuscript, which all authors approved.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–10, Supplementary Tables 1–4 and Supplementary Methods (PDF 977 kb)
Rights and permissions
About this article
Cite this article
Ortiz-Zapater, E., Pineda, D., Martínez-Bosch, N. et al. Key contribution of CPEB4-mediated translational control to cancer progression. Nat Med 18, 83–90 (2012). https://doi.org/10.1038/nm.2540
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.2540
This article is cited by
-
CircESRP1 enhances metastasis and epithelial–mesenchymal transition in endometrial cancer via the miR-874-3p/CPEB4 axis
Journal of Translational Medicine (2022)
-
The role of CPEB family proteins in the nervous system function in the norm and pathology
Cell & Bioscience (2021)
-
Molecular response to PARP1 inhibition in ovarian cancer cells as determined by mass spectrometry based proteomics
Journal of Ovarian Research (2021)
-
CPEB3-mediated MTDH mRNA translational suppression restrains hepatocellular carcinoma progression
Cell Death & Disease (2020)
-
LncRNA EWSAT1 upregulates CPEB4 via miR-330-5p to promote cervical cancer development
Molecular and Cellular Biochemistry (2020)