Abstract
Cancer-associated fibroblasts (CAFs) comprise the majority of the tumor bulk of pancreatic ductal adenocarcinomas (PDACs). Current efforts to eradicate these tumors focus predominantly on targeting the proliferation of rapidly growing cancer epithelial cells. We know that this is largely ineffective with resistance arising in most tumors following exposure to chemotherapy. Despite the long-standing recognition of the prominence of CAFs in PDAC, the effect of chemotherapy on CAFs and how they may contribute to drug resistance in neighboring cancer cells is not well characterized. Here, we show that CAFs exposed to chemotherapy have an active role in regulating the survival and proliferation of cancer cells. We found that CAFs are intrinsically resistant to gemcitabine, the chemotherapeutic standard of care for PDAC. Further, CAFs exposed to gemcitabine significantly increase the release of extracellular vesicles called exosomes. These exosomes increased chemoresistance-inducing factor, Snail, in recipient epithelial cells and promote proliferation and drug resistance. Finally, treatment of gemcitabine-exposed CAFs with an inhibitor of exosome release, GW4869, significantly reduces survival in co-cultured epithelial cells, signifying an important role of CAF exosomes in chemotherapeutic drug resistance. Collectively, these findings show the potential for exosome inhibitors as treatment options alongside chemotherapy for overcoming PDAC chemoresistance.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Stathis A, Moore MJ . Advanced pancreatic carcinoma: current treatment and future challenges. Nat Rev 2010; 7: 163–172.
Rahib L, Smith BD, Aizenberg R, Rosenzweig AB, Fleshman JM, Matrisian LM . Projecting cancer incidence and deaths to 2030: the unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res 2014; 74: 2913–2921.
Oettle H, Post S, Neuhaus P, Gellert K, Langrehr J, Ridwelski K et al. Adjuvant chemotherapy with gemcitabine vs observation in patients undergoing curative-intent resection of pancreatic cancer: a randomized controlled trial. JAMA 2007; 297: 267–277.
Kleeff J, Beckhove P, Esposito I, Herzig S, Huber PE, Lohr JM et al. Pancreatic cancer microenvironment. Int J Cancer 2007; 121: 699–705.
Chu GC, Kimmelman AC, Hezel AF, DePinho RA . Stromal biology of pancreatic cancer. J Cell Biochem 2007; 101: 887–907.
Hwang RF, Moore T, Arumugam T, Ramachandran V, Amos KD, Rivera A et al. Cancer-associated stromal fibroblasts promote pancreatic tumor progression. Cancer Res 2008; 68: 918–926.
Olive KP, Jacobetz MA, Davidson CJ, Gopinathan A, McIntyre D, Honess D et al. Inhibition of Hedgehog signaling enhances delivery of chemotherapy in a mouse model of pancreatic cancer. Science 2009; 324: 1457–1461.
Von Hoff DD, Ervin T, Arena FP, Chiorean EG, Infante J, Moore M et al. Increased survival in pancreatic cancer with nab-paclitaxel plus gemcitabine. N Engl J Med 2013; 369: 1691–1703.
Rhim AD, Oberstein PE, Thomas DH, Mirek ET, Palermo CF, Sastra SA et al. Stromal elements act to restrain, rather than support, pancreatic ductal adenocarcinoma. Cancer Cell 2014; 25: 735–747.
Valadi H, Ekstrom K, Bossios A, Sjostrand M, Lee JJ, Lotvall JO . Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat Cell Biol 2007; 9: 654–659.
Mathivanan S, Ji H, Simpson RJ . Exosomes: extracellular organelles important in intercellular communication. J Proteomics 2010; 73: 1907–1920.
Luga V, Zhang L, Viloria-Petit AM, Ogunjimi AA, Inanlou MR, Chiu E et al. Exosomes mediate stromal mobilization of autocrine Wnt-PCP signaling in breast cancer cell migration. Cell 2012; 151: 1542–1556.
Boelens Mirjam C, Wu Tony J, Nabet Barzin Y, Xu B, Qiu Y, Yoon T et al. Exosome transfer from stromal to breast cancer cells regulates therapy resistance pathways. Cell 159: 499–513.
Cheng L, Sharples RA, Scicluna BJ, Hill AF . Exosomes provide a protective and enriched source of miRNA for biomarker profiling compared to intracellular and cell-free blood. J Extracell Vesicles 2014; 3: 10.3402/jev.v3.23743.
Zhou W, Fong MY, Min Y, Somlo G, Liu L, Palomares MR et al. Cancer-secreted miR-105 destroys vascular endothelial barriers to promote metastasis. Cancer cell 2014; 25: 501–515.
Umezu T, Ohyashiki K, Kuroda M, Ohyashiki JH . Leukemia cell to endothelial cell communication via exosomal miRNAs. Oncogene 2013; 32: 2747–2755.
Kadera BE, Li L, Toste PA, Wu N, Adams C, Dawson DW et al. MicroRNA-21 in pancreatic ductal adenocarcinoma tumor-associated fibroblasts promotes metastasis. PLoS ONE 2013; 8: e71978.
Braicu C, Tomuleasa C, Monroig P, Cucuianu A, Berindan-Neagoe I, Calin GA . Exosomes as divine messengers: are they the Hermes of modern molecular oncology? Cell Death Differ 2015; 22: 34–45.
Chernyshev VS, Rachamadugu R, Tseng YH, Belnap DM, Jia Y, Branch KJ et al. Size and shape characterization of hydrated and desiccated exosomes. Anal Bioanal Chem 2015; 407: 3285–3301.
Caby MP, Lankar D, Vincendeau-Scherrer C, Raposo G, Bonnerot C . Exosomal-like vesicles are present in human blood plasma. Int Immunol 2005; 17: 879–887.
Svensson KJ, Christianson HC, Wittrup A, Bourseau-Guilmain E, Lindqvist E, Svensson LM et al. Exosome uptake depends on ERK1/2-heat shock protein 27 signaling and lipid Raft-mediated endocytosis negatively regulated by caveolin-1. J Biol Chem 2013; 288: 17713–17724.
Hwang WL, Jiang JK, Yang SH, Huang TS, Lan HY, Teng HW et al. MicroRNA-146a directs the symmetric division of Snail-dominant colorectal cancer stem cells. Nat Cell Biol 2014; 16: 268–280.
Essandoh K, Yang L, Wang X, Huang W, Qin D, Hao J et al. Blockade of exosome generation with GW4869 dampens the sepsis-induced inflammation and cardiac dysfunction. Biochim Biophys Acta 2015; 1852: 2362–2371.
Arora S, Bhardwaj A, Singh S, Srivastava SK, McClellan S, Nirodi CS et al. An undesired effect of chemotherapy: gemcitabine promotes pancreatic cancer cell invasiveness through reactive oxygen species-dependent, nuclear factor kappaB- and hypoxia-inducible factor 1alpha-mediated up-regulation of CXCR4. J Biol Chem 2013; 288: 21197–21207.
Banerjee S, Kaseb AO, Wang Z, Kong D, Mohammad M, Padhye S et al. Antitumor activity of gemcitabine and oxaliplatin is augmented by thymoquinone in pancreatic cancer. Cancer Res. 2009; 69: 5575–5583.
Arlt A, Gehrz A, Muerkoster S, Vorndamm J, Kruse ML, Folsch UR et al. Role of NF-kappaB and Akt/PI3K in the resistance of pancreatic carcinoma cell lines against gemcitabine-induced cell death. Oncogene 2003; 22: 3243–3251.
Banerjee S, Zhang Y, Ali S, Bhuiyan M, Wang Z, Chiao PJ et al. Molecular evidence for increased antitumor activity of gemcitabine by genistein in vitro and in vivo using an orthotopic model of pancreatic cancer. Cancer Res. 2005; 65: 9064–9072.
Quint K, Tonigold M, Di Fazio P, Montalbano R, Lingelbach S, Rückert F et al. Pancreatic cancer cells surviving gemcitabine treatment express markers of stem cell differentiation and epithelial-mesenchymal transition. Int J Oncol 2012; 41: 2093–2102.
Namba T, Kodama R, Moritomo S, Hoshino T, Mizushima T . Zidovudine, an anti-viral drug, resensitizes gemcitabine-resistant pancreatic cancer cells to gemcitabine by inhibition of the Akt-GSK3beta-Snail pathway. Cell Death Dis 2015; 6: e1795.
Kaufhold S, Bonavida B . Central role of Snail1 in the regulation of EMT and resistance in cancer: a target for therapeutic intervention. J Exp Clin Cancer Res 2014; 33: 62.
Lee TH, Chennakrishnaiah S, Audemard E, Montermini L, Meehan B, Rak J . Oncogenic ras-driven cancer cell vesiculation leads to emission of double-stranded DNA capable of interacting with target cells. Biochem Biophys Res Commun 2014; 451: 295–301.
Hu Y, Yan C, Mu L, Huang K, Li X, Tao D et al. Fibroblast-derived exosomes contribute to chemoresistance through priming cancer stem cells in colorectal cancer. PLoS One 2015; 10: e0125625.
Boelens MC, Wu Tony, J, Nabet BY, Xu B, Qiu Y, Yoon T et al. Exosome transfer from stromal to breast cancer cells regulates therapy resistance pathways. Cell 2014; 159: 499–513.
Ray K . Pancreatic cancer: Pancreatic cancer exosomes prime the liver for metastasis. Nat Rev 2015; 12: 371.
Zhang L, Zhang S, Yao J, Lowery FJ, Zhang Q, Huang WC et al. Microenvironment-induced PTEN loss by exosomal microRNA primes brain metastasis outgrowth. Nature 2015; 527: 100–104.
Hoshino A, Costa-Silva B, Shen TL, Rodrigues G, Hashimoto A, Tesic Mark M et al. Tumour exosome integrins determine organotropic metastasis. Nature 2015; 527: 329–335.
Arensman MD, Kovochich AN, Kulikauskas RM, Lay AR, Yang PT, Li X et al. WNT7B mediates autocrine Wnt/beta-catenin signaling and anchorage-independent growth in pancreatic adenocarcinoma. Oncogene 2014; 33: 899–908.
Sun N, Johnson J, Stack MS, Szajko J, Sander C, Rebuyon R et al. Nanoparticle analysis of cancer cells by light transmission spectroscopy. Anal Biochem 2015; 484: 58–65.
Arumugam T, Ramachandran V, Fournier KF, Wang H, Marquis L, Abbruzzese JL et al. Epithelial to mesenchymal transition contributes to drug resistance in pancreatic cancer. Cancer Res. 2009; 69: 5820–5828.
Gifford JB, Huang W, Zeleniak AE, Hindoyan A, Wu H, Donahue TR et al. Expression Of GRP78, master regulator of the unfolded protein response, increases chemoresistance in pancreatic ductal adenocarcinoma. Mol Cancer Ther 2016; 15: 1043–1052.
Acknowledgements
We acknowledge Dr Robert Stahelin of the Indiana University School of Medicine for generously allowing us to use his particle analyzer and ultracentrifuge, Dr Niranjan Awasthi of the Indiana University School of Medicine–South Bend for helpful discussions and Dr Steven Ruggiero of the University of Notre Dame for allowing us to perform light transmission spectroscopy in his lab. This research was funded by the Indiana CTSI and Harper Cancer Research Institute of Notre Dame.
Financial Information: R Hill was awarded financial support from the Walther Cancer Foundation and the Joseph D Boyle Memorial Fund. Work by ML Fishel was supported by grants from the National Institutes of Health, NCI CA167291, with additional support from the Biomedical Research Grant and in part by Jeff Gordon Children’s Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Richards, K., Zeleniak, A., Fishel, M. et al. Cancer-associated fibroblast exosomes regulate survival and proliferation of pancreatic cancer cells. Oncogene 36, 1770–1778 (2017). https://doi.org/10.1038/onc.2016.353
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2016.353
This article is cited by
-
Cancer associated fibroblasts serve as an ovarian cancer stem cell niche through noncanonical Wnt5a signaling
npj Precision Oncology (2024)
-
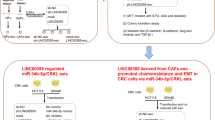
Cancer-associated fibroblast exosome LINC00355 promotes epithelial-mesenchymal transition and chemoresistance in colorectal cancer through the miR-34b-5p/CRKL axis
Cancer Gene Therapy (2024)
-
NNT-AS1 in CAFs-derived exosomes promotes progression and glucose metabolism through miR-889-3p/HIF-1α in pancreatic adenocarcinoma
Scientific Reports (2024)
-
miRNAs in pancreatic cancer progression and metastasis
Clinical & Experimental Metastasis (2024)
-
Nanomaterial Assisted Exosome Analysis Using Mass Spectrometry
Chemical Research in Chinese Universities (2024)