Abstract
Background
Dysregulated lipid metabolism is associated with more aggressive pathology and poorer prognosis in prostate cancer (PC). The primary aim of the study is to assess the relationship between the plasma lipidome and clinical outcomes in localised and metastatic PC. The secondary aim is to validate a prognostic circulating 3-lipid signature specific to metastatic castration-resistant PC (mCRPC).
Patients and methods
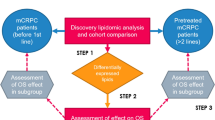
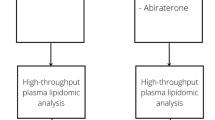
Comprehensive lipidomic analysis was performed on pre-treatment plasma samples from men with localised PC (N = 389), metastatic hormone-sensitive PC (mHSPC)(N = 44), or mCRPC (validation cohort, N = 137). Clinical outcomes from our previously published mCRPC cohort (N = 159) that was used to derive the prognostic circulating 3-lipid signature, were updated. Associations between circulating lipids and clinical outcomes were examined by Cox regression and latent class analysis.
Results
Circulating lipid profiles featuring elevated levels of ceramide species were associated with metastatic relapse in localised PC (HR 5.80, 95% CI 3.04–11.1, P = 1 × 10−6), earlier testosterone suppression failure in mHSPC (HR 3.70, 95% CI 1.37–10.0, P = 0.01), and shorter overall survival in mCRPC (HR 2.54, 95% CI 1.73–3.72, P = 1 × 10−6). The prognostic significance of circulating lipid profiles in localised PC was independent of standard clinicopathological and metabolic factors (P < 0.0002). The 3-lipid signature was verified in the mCRPC validation cohort (HR 2.39, 95% CI 1.63–3.51, P = 1 × 10−5).
Conclusions
Elevated circulating ceramide species are associated with poorer clinical outcomes across the natural history of PC. These clinically actionable lipid profiles could be therapeutically targeted in prospective clinical trials to potentially improve PC outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin. 2018;68:394–424.
Sartor O, de Bono JS. Metastatic Prostate Cancer. N Engl J Med. 2018;378:645–57.
Iyengar NM, Gucalp A, Dannenberg AJ, Hudis CA. Obesity and Cancer Mechanisms: tumor Microenvironment and Inflammation. J Clin Oncol. 2016;34:4270–6.
Allott EH, Masko EM, Freedland SJ. Obesity and prostate cancer: weighing the evidence. Eur Urol. 2013;63:800–9.
Wu X, Daniels G, Lee P, Monaco ME. Lipid metabolism in prostate cancer. Am J Clin Exp Urol. 2014;2:111–20.
Zadra G, Ribeiro CF, Chetta P, Ho Y, Cacciatore S, Gao X, et al. Inhibition of de novo lipogenesis targets androgen receptor signaling in castration-resistant prostate cancer. Proc Natl Acad Sci USA. 2019;116:631–40.
Allott EH, Howard LE, Cooperberg MR, Kane CJ, Aronson WJ, Terris MK, et al. Serum lipid profile and risk of prostate cancer recurrence: results from the SEARCH database. Cancer Epidemiol Biomark Prev. 2014;23:2349–56.
Wu S-Y, Fang S-C, Shih H-J, Wen Y-C, Shao Y-HJ. Mortality associated with statins in men with advanced prostate cancer treated with androgen deprivation therapy. Eur J Cancer. 2019;112:109–17.
Van Rompay MI, Solomon KR, Nickel JC, Ranganathan G, Kantoff PW, McKinlay JB. Prostate cancer incidence and mortality among men using statins and non-statin lipid-lowering medications. Eur J Cancer. 2019;112:118–26.
Raval AD, Thakker D, Negi H, Vyas A, Salkini MW. Association between statins and clinical outcomes among men with prostate cancer: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2016;19:151–62.
Quehenberger O, Dennis EA. The human plasma lipidome. N Engl J Med. 2011;365:1812–23.
Lin HM, Mahon KL, Weir JM, Mundra PA, Spielman C, Briscoe K, et al. A distinct plasma lipid signature associated with poor prognosis in castration-resistant prostate cancer. Int J Cancer. 2017;141:2112–20.
Summers SA, Chaurasia B, Holland WL. Metabolic Messengers: ceramides. Nat Metab. 2019;1:1051–8.
Laaksonen R, Ekroos K, Sysi-Aho M, Hilvo M, Vihervaara T, Kauhanen D, et al. Plasma ceramides predict cardiovascular death in patients with stable coronary artery disease and acute coronary syndromes beyond LDL-cholesterol. Eur Heart J. 2016;37:1967–76.
Vykoukal J, Fahrmann JF, Gregg JR, Tang Z, Basourakos S, Irajizad E, et al. Caveolin-1-mediated sphingolipid oncometabolism underlies a metabolic vulnerability of prostate cancer. Nat Commun. 2020;11:4279.
Kohli M, Tan W, Zheng T, Wang A, Montesinos C, Wong C, et al. Clinical and genomic insights into circulating tumor DNA-based alterations across the spectrum of metastatic hormone-sensitive and castrate-resistant prostate cancer. EBioMedicine. 2020;54:102728.
Huynh K, Barlow CK, Jayawardana KS, Weir JM, Mellett NA, Cinel M, et al. High-Throughput Plasma Lipidomics: detailed Mapping of the Associations with Cardiometabolic Risk Factors. Cell Chem Biol. 2019;26:71–84.e74.
Linzer DA, Lewis JB. poLCA: an R Package for Polytomous Variable Latent Class Analysis. J Stat Softw. 2011;42:1–29.
Xie W, Regan MM, Buyse M, Halabi S, Kantoff PW, Sartor O, et al. Metastasis-Free Survival Is a Strong Surrogate of Overall Survival in Localized Prostate Cancer. J Clin Oncol. 2017;35:3097–104.
Hannun YA, Obeid LM. Principles of bioactive lipid signalling: lessons from sphingolipids. Nat Rev Mol Cell Biol. 2008;9:139–50.
Meikle PJ, Wong G, Tan R, Giral P, Robillard P, Orsoni A, et al. Statin action favors normalization of the plasma lipidome in the atherogenic mixed dyslipidemia of MetS: potential relevance to statin-associated dysglycemia. J Lipid Res. 2015;56:2381–92.
Mundra PA, Barlow CK, Nestel PJ, Barnes EH, Kirby A, Thompson P. et al. Large-scale plasma lipidomic profiling identifies lipids that predict cardiovascular events in secondary prevention. JCI Insight. 2018;3:e121326.
Wiesner P, Leidl K, Boettcher A, Schmitz G, Liebisch G. Lipid profiling of FPLC-separated lipoprotein fractions by electrospray ionization tandem mass spectrometry. J Lipid Res. 2009;50:574–85.
Lightle S, Tosheva R, Lee A, Queen-Baker J, Boyanovsky B, Shedlofsky S, et al. Elevation of ceramide in serum lipoproteins during acute phase response in humans and mice: role of serine-palmitoyl transferase. Arch Biochem Biophys. 2003;419:120–8.
Cerami E, Gao J, Dogrusoz U, Gross BE, Sumer SO, Aksoy BA, et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Disco. 2012;2:401–4.
Llorente A, Skotland T, Sylvanne T, Kauhanen D, Rog T, Orlowski A, et al. Molecular lipidomics of exosomes released by PC-3 prostate cancer cells. Biochim Biophys Acta. 2013;1831:1302–9.
Malavaud B, Pchejetski D, Mazerolles C, de Paiva GR, Calvet C, Doumerc N, et al. Sphingosine kinase-1 activity and expression in human prostate cancer resection specimens. Eur J Cancer. 2010;46:3417–24.
Seelan RS, Qian C, Yokomizo A, Bostwick DG, Smith DI, Liu W. Human acid ceramidase is overexpressed but not mutated in prostate cancer. Genes Chromosom Cancer. 2000;29:137–46.
Ogretmen B. Sphingolipid metabolism in cancer signalling and therapy. Nat Rev Cancer. 2018;18:33–50.
van der Weyden L, Arends MJ, Campbell AD, Bald T, Wardle-Jones H, Griggs N, et al. Genome-wide in vivo screen identifies novel host regulators of metastatic colonization. Nature. 2017;541:233–6.
Santos WL, Lynch KR. Drugging sphingosine kinases. ACS Chem Biol. 2015;10:225–33.
Shah C, Yang G, Lee I, Bielawski J, Hannun YA, Samad F. Protection from high fat diet-induced increase in ceramide in mice lacking plasminogen activator inhibitor 1. J Biol Chem. 2008;283:13538–48.
Nagahashi M, Yamada A, Katsuta E, Aoyagi T, Huang WC, Terracina KP, et al. Targeting the SphK1/S1P/S1PR1 Axis That Links Obesity, Chronic Inflammation, and Breast Cancer Metastasis. Cancer Res. 2018;78:1713–25.
Hilvo M, Simolin H, Metso J, Ruuth M, Oorni K, Jauhiainen M, et al. PCSK9 inhibition alters the lipidome of plasma and lipoprotein fractions. Atherosclerosis. 2018;269:159–65.
Tarasov K, Ekroos K, Suoniemi M, Kauhanen D, Sylvanne T, Hurme R, et al. Molecular lipids identify cardiovascular risk and are efficiently lowered by simvastatin and PCSK9 deficiency. J Clin Endocrinol Metab. 2014;99:E45–52.
Kasumov T, Solomon TP, Hwang C, Huang H, Haus JM, Zhang R, et al. Improved insulin sensitivity after exercise training is linked to reduced plasma C14:0 ceramide in obesity and type 2 diabetes. Obes (Silver Spring). 2015;23:1414–21.
Clendinen CS, Gaul DA, Monge ME, Arnold RS, Edison AS, Petros JA, et al. Preoperative Metabolic Signatures of Prostate Cancer Recurrence Following Radical Prostatectomy. J Proteome Res. 2019;18:1316–27.
Snider AJ, Seeds MC, Johnstone L, Snider JM, Hallmark B, Dutta R, et al. Identification of Plasma Glycosphingolipids as Potential Biomarkers for Prostate Cancer (PCa) Status. Biomolecules. 2020;10:1393.
Acknowledgements
We gratefully acknowledge Maurene Giles and Cassandra Gordon (Australian Prostate Cancer BioResource) for collection and annotation of clinical follow-up data for the localised PC cohort; Anne-Maree Haynes (Garvan Institute of Medical Research), Lisa Graham (Chris O’Brien Lifehouse), Jessica Savage and Kayla Bremert (South Australian node coordinators of the Australian Prostate Cancer BioResource), the PRIMe consortium, and research nurses for collection of blood specimens and clinical data; Alexander Smith and Gavriel Olshansky (Baker Heart and Diabetes Institute) for their useful discussion on statistical analysis; our consumer representative Tony Maxwell for reviewing the paper; and the patients for their participation.
Funding
National Health and Medical Research Council of Australia (GNT0614296), Cancer Institute New South Wales (10/TPG/1-04, 2018/TPG001), Australian Prostate Cancer Research Centre-New South Wales, Australian Department of Health and Aging, the Movember Foundation and the Prostate Cancer Foundation of Australia (Revolutionary Team Award MRTA3), Cancer Council New South Wales (PG 10-01), Cancer Council South Australia (Beat Cancer Project Principal Cancer Research Fellowship, (PRF1117) to LMB), The Victorian Government’s Operational Infrastructure Support Program, National Institutes of Health grant award to MK (RO1-CA212097).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
AAA: Consultant—Astellas, Janssen, Novartis; Speakers Bureau—Astellas, Janssen, Novartis, Amgen; Honoraria—Astellas, Janssen, Novartis, Tolmar, Amgen, Pfizer, Telix; Scientific Advisory Board—Astellas, Novartis, Sanofi, Astra Zeneca, Tolmar, Pfizer, Telix; Research Funding—Astellas, Merck Serono, Bristol Myers Squibb (institutional), Astra Zeneca (institutional), Aptevo Therapeutics (institutional), Glaxo Smith Kline (institutional), Pfizer (institutional), MedImmune (institutional), Astellas (institutional), SYNthorx (institutional), Bionomics (institutional), Sanofi Aventis (institutional), Novartis (institutional). LGH: Research funding—Astellas; Travel sponsorship—Janssen, Pfizer; Honoraria—Imagion Biosystems. All remaining authors have declared no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Lin, HM., Huynh, K., Kohli, M. et al. Aberrations in circulating ceramide levels are associated with poor clinical outcomes across localised and metastatic prostate cancer. Prostate Cancer Prostatic Dis 24, 860–870 (2021). https://doi.org/10.1038/s41391-021-00338-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-021-00338-z
This article is cited by
-
PCPro: a clinically accessible, circulating lipid biomarker signature for poor-prognosis metastatic prostate cancer
Prostate Cancer and Prostatic Diseases (2023)
-
Untargeted lipidomics reveal association of elevated plasma C18 ceramide levels with reduced survival in metastatic castration-resistant prostate cancer patients
Scientific Reports (2023)
-
Extensive metabolic consequences of human glycosyltransferase gene knockouts in prostate cancer
British Journal of Cancer (2023)
-
Combined impact of lipidomic and genetic aberrations on clinical outcomes in metastatic castration-resistant prostate cancer
BMC Medicine (2022)