Abstract
Schlager mice (BPH/2J) are hypertensive due to a greater contribution of the sympathetic nervous system (SNS) and renin-angiotensin system (RAS). The kidneys of BPH/2J are hyper-innervated suggesting renal nerves may contribute to the hypertension. We therefore determined the effect of bilateral renal denervation (RD) on hypertension in BPH/2J. Mean arterial pressure (MAP) was measured by radiotelemetry before and for 3 weeks after RD in BPH/2J and BPN/3J. The effects of pentolinium and enalaprilat were examined to determine the contribution of the SNS and RAS, respectively. After 3 weeks, MAP was −10.9 ± 2.1 mmHg lower in RD BPH/2J compared to baseline and −2.1 ± 2.2 mmHg in sham BPH/2J (P < 0.001, n = 8–10). RD had no effect in BPN/3J (P > 0.1). The depressor response to pentolinium was greater in BPH/2J than BPN/3J, but in both cases the response in RD mice was similar to sham. Enalaprilat decreased MAP more in RD BPH/2J compared to sham (−12 vs −3 mmHg, P < 0.001) but had no effect in BPN/3J. RD reduced renal noradrenaline in both strains but more so in BPH/2J. RD reduced renin mRNA and protein, but not plasma renin in BPH/2J to levels comparable with BPN/3J mice. We conclude that renal nerves contribute to hypertension in BPH mice as RD induced a sustained fall in MAP, which was associated with a reduction of intrarenal renin expression. The lack of inhibition of the depressor effects of pentolinium and enalaprilat by RD suggests that vasoconstrictor effects of the SNS or RAS are not involved.
Similar content being viewed by others
Introduction
BPH/2J mice are a genetic model of hypertension developed by Schlager in the 1970s and selected for their elevated blood pressure after crossing 8 normotensive strains [1]. BPN/3J mice are a normotensive strain obtained from the same base population as BPH/2J mice and used as their controls. BPH/2J mice are suggested to have a neurogenic form of hypertension due to greater activity of the sympathetic nervous system (SNS). This was first demonstrated when the mean arterial pressure (MAP) of BPH/2J mice was reduced by sympathetic ganglion blockade to a level similar to that of normotensive BPN/3J mice [2]. Elevated MAP in BPH/2J mice was associated with an increase in central nervous system neuronal activity, shown by immunohistochemistry to be 1.7-fold greater in the medial amygdala (MeAm) of BPH/2J mice than in BPN/3J mice [2]. Lesions in the MeAm reduced MAP of BPH/2J mice to a level toward that of the BPN/3J strain, confirming the contribution of the MeAm to SNS overactivity and the hypertension of BPH/2J mice [3]. Furthermore, BPH/2J mice have greater renal sympathetic innervation compared with BPN/3J mice [4]. Recently, the renin-angiotensin system (RAS) was implicated in the hypertension of BPH/2J mice, with evidence that renal renin (Ren1) mRNA expression was greater in BPH/2J mice compared with BPN/3J mice [4]. This increase in renin mRNA expression was correlated with a greater depressor response to the ganglion inhibitor pentolinium. Thus, we hypothesized that exaggerated renal sympathetic activity contributes to elevated MAP in BPH/2J mice at least partly through a mechanism that includes greater renal renin expression. Renal denervation (RD) of BPH/2J mice is therefore likely to reduce MAP effectively in this neurogenic hypertensive strain. RD is known to reduce MAP in a number of other experimental animal models of hypertension such as the spontaneously hypertensive rat (SHR) [5], DOCA saline hypertension [6] but not in Dahl salt sensitive hypertension [7], mild DOCA salt hypertension [8], or Angiotensin II hypertension [9]. In patients with resistant hypertension, catheter-based RD has received much attention [10, 11] especially more recently with the trial that showed its effectiveness in hypertensive patients that had been withdrawn from therapy [12]. Thus, although there have been very many renal denervation studies reported, very few have examined the underlying mechanism. The aim of this study was to determine the effects of bilateral RD on MAP in BPH/2J and BPN/3J mice. To assess the relative contributions of the SNS and RAS in the maintenance of BP following RD, pentolinium and the angiotensin-converting enzyme (ACE) inhibitor enalaprilat respectively were used. Furthermore, the effect of RD on renal renin mRNA and protein expression was determined.
Methods
Animals
Experiments were performed on normotensive BPN/3J (n = 18) and genetically hypertensive BPH/2J (n = 12) adult male mice with an average age of 14 weeks at the time of the first surgery. All experiments were approved by the Alfred Medical Research Education Precinct Animal Ethics Committee and conducted in accordance with the Australian Code of Practice for Scientific Use of Animals. Animals were housed individually under conditions of light (12 h on and off) and temperature control with environmental enrichment and free access to food and water. See online data supplement for surgery and experimental sequence of events (Supplementary Figure 1).
Preliminary surgery
Mice underwent two surgical procedures under isoflurane open circuit anaesthesia (4% induction and 1.5–2% maintenance in oxygen; Forthane, Abbott Australasia, Botany, NSW, Australia). Carprofen (5 mg/kg, subcutaneously, Rimadyl, Pfizer Australia, West Ryde, NSW, Australia) and local bupivacaine (2 mg/kg, AstraZeneca, North Ryde, NSW, Australia) were given before surgery and carprofen was given again 24 h post surgery for analgesia. In the first operation, a BP radiotelemetry transmitter (model TA11PA-C10; Data Sciences International, St Paul, MN, USA) was implanted [13]. The catheter of the telemetry device was inserted into the left carotid artery and the transmitter was positioned subcutaneously along the right flank. Three weeks following telemetry surgery, bilateral RD was conducted as described previously [14]. Before surgery, mice also received atropine (1.2 mg/kg, intraperitoneally, Sigma, St Louis, USA) to reduce secretions. Kidneys were exposed by an abdominal midline incision. All visible renal nerves were cut, renal vessels were stripped, painted with a solution of 10% phenol in absolute ethanol and enclosed for 3 min by a sterile gelatine sponge (1 × 4 mm) soaked with the 10% phenol solution. The gelatine sponge was removed and surrounding tissue was rinsed with normal saline (Baxter Healthcare, Old Toongabbie, NSW, Australia). The muscle and skin layers were separately sutured, and the mice received Hartmann’s solution (0.3 mL/mouse, subcutaneously) before being returned to their home cages. Sham-treated mice underwent surgery to expose the kidneys, but phenol was not applied.
Cardiovascular measurements
After a 10-day recovery period from telemetry surgery, baseline cardiovascular parameters and locomotor activity were recorded over 72 h. Following RD, cardiovascular parameters and locomotor activity were recorded over 24 h on 6 occasions within 3 weeks (days 3, 6, 9, 12, 18 and 21 post surgery). All recordings of systolic arterial pressure (SAP), diastolic arterial pressure (DAP), calculated MAP, heart rate (HR), and locomotor activity were obtained in freely moving mice in their home cage. The recordings were sampled at 1000 Hz using an analogue-to-digital data acquisition card (National Instruments 6024E, Austin, Texas, USA) [15]. The beat-to-beat data were detected on line and analysed later using a program written in the LabVIEW programming language (National Instruments, Austin, Texas, USA).
Cardiovascular variability and the cardiac baroreceptor sensitivity
Spectral analysis of cardiovascular variability and the baroreceptor HR reflex gain were measured during the active dark period as described previously in sham and RD BPN/3J and BPH/2J mice (n = 6–8) [3]. The auto- and cross-power spectra were determined for multiple 50% overlapping segments of MAP and HR using a Fast Fourier transform. The cardiac baroreflex sensitivity was estimated as the average value of the transfer gain in the frequency band between 0.3 and 0.5 Hz. Baroreflex slope was considered significant if the coherence between MAP and HR across several overlapping segments in the analysed frequency band was >0.4. Data periods with low locomotor activity were chosen (4 from each circadian period) from 48-hour recordings minimizing the influence of physical activity.
Assessment of cardiovascular reactivity in response to stress tests
A series of behavioural tests were conducted during the inactive period 2 weeks after RD surgery (days 12–17 post surgery) in order to test whether activation of the SNS had been affected. Following a 60 min baseline recording, animals were exposed to one of three stimuli (restraint stress, dirty cage-switch stress and feeding), for 60 min on three separate days [3]. Restraint stress involved guiding the mouse into a cylindrical Plexiglas restrainer with a sliding back plate to confine the animal. Immobilization minimizes the contribution of locomotor activity to cardiovascular responses to stress. Dirty cage-switch stress involved placing the mouse in a cage previously occupied by another male mouse. This aversive stressor has been demonstrated to induce sustained pressor responses as well as increased locomotor activity [16]. Feeding stress involved presenting palatable food (pieces of almond) to mice that had been fasted overnight and observing the eating patterns each min during the 60 min period.
Cardiovascular response to ACE inhibition and ganglion blockade
Following a 30 min baseline recording, mice were administered the ACE inhibitor enalaprilat (1 mg/kg intraperitoneal; Merck & Co, Keniworth, NJ, USA), followed 40 min later by the ganglion blocker, pentolinium (5 mg/kg, intraperitoneal; Sigma-Aldrich, Castle Hill, NSW Australia) as described previously [3]. ACE inhibition prior to ganglion blockade has been shown to reduce the compensatory response of the RAS following ganglion blockade, unmasking the full contribution of the SNS in BPH/2J mice [4]. The cardiovascular responses were evaluated during both the light (inactive) period and the dark (active) period, on separate days, 2 weeks after RD surgery.
Tissue and blood collection and analysis
Three weeks following RD surgery, mice received an overdose of sodium pentobarbitone (Lethobarb; Virbac Animal Health, New South Wales, Australia) 2 h after turning off the lights. A blood sample was collected by cardiac puncture and plasma and kidneys were snap frozen in liquid nitrogen and stored at −80 °C. Noradrenaline content was later measured in kidneys (n = 6–10 per group) and results were expressed in pg of noradrenaline per g of wet tissue as previously described [17]. Renal RNA was extracted and Ren1 mRNA abundance was measured in BPH/2J and BPN/3J mouse kidneys (n = 7–9 per group), following removal during the dark (active) period, as we previously described [4]. Data from left and right kidneys were averaged.
Renal protein was extracted from the kidney by the use of RIPA buffer (Sigma-Aldrich) and 1% Halt Protease & Phosphatase Inhibitor Cocktail (Thermo Scientific, Scorseby, Victoria, Australia). Renal protein was quantified using DCTM Protein Assay and a bovine serum albumin standard (BioRad, Hercules, CA, USA). Mouse plasma collected in EDTA tubes (1:10 dilution) and renal protein (500 µg) were used to determine Ren1 protein with the Mouse Renin1 (Ren1) ELISA kit (Thermo Scientific) according to the supplier, in an EnSpire™ Multimode Plate Reader (PerkinElmer, Glen Waverley, Victoria Australia). Intra-assay coefficients of variability were calculated and only those less than 15% variability were accepted. The overall variability for the plasma plate was 3% and for the renal protein plate 3.8%.
Data analysis
Data were collected over 24-hour periods and were also assessed during the 12 h of lights on (inactive period) and lights off (active period). Responses to the different stressors were calculated by the difference between the 60-min baseline period and the 60-min stimulus period. The response to enalaprilat was represented by the difference between the baseline period (30 min recording before treatment) and that recorded 20–30 min after treatment. To calculate the effect of pentolinium, the 30-min period following enalaprilat injection was used as the control period and compared with the response 10–20 min after pentolinium injection.
Data are expressed as mean ± SEM and were analysed by split plot repeated measures analysis of variance, which was a mixed model allowing for within-animal and between-animal (group) contrasts. Comparisons used were Pstrain, which was BPH/2J vs BPN/3J, PRD which was sham vs RD and Pbaseline comparing the effect of denervation or sham surgery against baseline. Type 1 error was controlled using Bonferroni adjustment to the probability threshold and Greenhouse-Geisser correction to reduce inflated residual degree of freedom [18]. A probability of P < 0.05 was considered significant.
Results
Baseline cardiovascular measurements
MAP and HR, measured over 24 h, were 17% and 28% higher, respectively, in BPH/2J mice compared with BPN/3J mice (both Pstrain < 0.001, Table 1, baseline pooled from sham and RD groups). Locomotor activity was 1.5-fold greater in BPH/2J mice (Pstrain = 0.02, Table 1). During the dark (active) period, MAP and HR in BPH/2J mice were 21% and 33% greater, respectively (both Pstrain < 0.001), and locomotor activity was 1.9-fold greater, (Pstrain < 0.001) than in BPN/3J mice (Table 1). A similar pattern was observed in MAP and HR during the light (inactive) period but the differences between strains were smaller. MAP and HR were 13% and 23% greater, respectively, in BPH/2J compared to BPN/3J mice (Pstrain < 0.001) but locomotor activity was similar in the 2 strains (Pstrain = 0.99, Table 1). BPN/3J mice were heavier than BPH/2J mice by 4.1 g (27.9 vs 23.8 g, n = 16 and n = 18, Pstrain < 0.001), which is similar to our previous findings [19].
Effects of RD on cardiovascular, locomotor and body weight measurements
After RD, MAP in BPH/2J mice, averaged over 3 weeks, was 8.5 ± 0.8 mmHg lower than baseline (Pbaseline < 0.001) compared to sham-treated mice in which MAP remained similar to baseline (Pbaseline = 0.86, Fig. 1). The reduction was evident by day 3 and remained stable from day 6 to the end of the experiment on day 21 (Fig. 1). There was no detected change from baseline MAP over the 3 weeks after sham with the final 3-week reduction being 10.9 ± 2.1 mmHg lower in RD BPH/2J compared to 2.1 ± 2.2 mmHg lower in sham BPH/2J. RD had no effect in BPN/3J mice over the 3-week period (Pbaseline > 0.1, Fig. 2). Thus the effect of RD was markedly greater in BPH/2J than in BPN/3J mice (Pstrain < 0.001).
Line graphs show time course of changes in average 24-hour MAP, heart rate (HR), locomotor activity and body weight from baseline during the 3 weeks following renal denervation (RD, closed symbol, n = 10) or sham surgery (open symbol, n = 8) in genetically hypertensive BPH/2J mice. Histograms are mean change ± SEM from baseline over 3 weeks post denervation (RD, filled bars) or post sham surgery (open bars) in BPH/2J mice and were analysed by split plot analysis of variance. Error bars indicate between animal variance. #P < 0.05 and ###P < 0.001 for comparison of 3-week average with baseline, ***P < 0.001 for comparison of RD with sham group
Line graphs show time course of changes in average 24-hour MAP, heart rate (HR), locomotor activity and body weight from baseline during the 3 weeks following renal denervation (RD, closed symbol) or sham surgery (open symbol) in normotensive BPN/3J mice. Histograms are mean change ± SEM from baseline over 3 weeks post denervation (RD, filled bars, n = 7) or post sham surgery (open bars, n = 9) in BPN/3J mice and were analysed by split plot analysis of variance. Error bars indicate between animal variance. ##P < 0.01 for comparison of 3-week average with baseline, *P < 0.05 for comparison of RD with sham group
HR fell by −38 ± 5 b/min in BPH/2J mice in the 3 weeks following RD (Pbaseline < 0.001) but was also lower than baseline after sham surgery (−31 ± 5 b/min, Pbaseline < 0.001, Fig. 1). In BPN/3J mice, HR was elevated from baseline following denervation (+18 ± 5 b/min, Pbaseline = 0.027) but there was no change following sham surgery (Pbaseline = 0.42, Fig. 2).
In BPH/2J mice there was a modest reduction in locomotor activity level from baseline following RD (Pbaseline = 0.011) but not sham treatment and there was no effect on activity following either sham or RD in BPN/3J mice (Pbaseline > 0.1).
There was no difference in the body weight change over the 3 weeks in sham or denervated BPN/3J mice (Pstrain = 0.67, Fig. 2). Averaged over the 3 weeks, there was a modest decrease in body weight in denervated BPH/2J mice particularly between day 3 and 9 that was not observed in sham treated mice (Pstrain = 0.013, Fig. 1). By day 21 there was no difference in the body weight between the sham or RD BPH/2J mice (Fig. 1).
Effects of RD on circadian pattern of cardiovascular measurements
As the extent of the hypotensive effects of RD were relatively constant over the 3 weeks, the average of the 24-hour recordings of MAP, HR and activity during this time were compared to baseline recordings but shown by hourly average to show more clearly the nocturnal pattern (Figs. 3 and 4). BPH/2J showed markedly higher levels of MAP, HR and activity during the active (dark) period compared to the inactive (light) period. By contrast BPN/3J exhibited much lesser day night differences in all variables.
Line graphs show hourly averages of mean arterial pressure (MAP), heart rate (HR) and locomotor activity during the dark (active, outer panels) and light (inactive, middle panel) periods. Data are from BPN/3J (left, grey circle, n = 7) and BPH/2J (right, black square, n = 10) mice at baseline (pre-surgery, open symbols) and following renal denervation (RD) surgery (average over the 3 weeks, closed symbols). Histograms are mean change ± SEM from baseline during the dark period (hatched) and the light (inactive) period (open) over the 3 weeks of the experiment and were analysed by split plot analysis of variance to determine whether changes from baseline were similar during the light and dark period
Line graphs show hourly averages of mean arterial pressure (MAP), heart rate (HR) and locomotor activity during the dark (active, outer panels) and light (inactive, middle panel) periods. Data are from BPN/3J (left, grey circle, n = 9) and BPH/2J (right, black square, n = 8) mice at baseline (pre-surgery, open symbols) and following sham surgery (average over the 3 weeks, closed symbols). Histograms are mean change ± SEM from baseline during the dark period (hatched) and the light (inactive) period (open) over the 3 weeks of the experiment and were analysed by split plot analysis of variance to determine whether changes from baseline were similar during the light and dark period
We determined whether the changes occurring over the 3 weeks were evident in both the light and dark period (Figs. 3 and 4). The hypotensive effect of RD were equally evident in BPH/2J mice during both active (dark) and inactive (light) periods (Effect between day night P = 0.40, Fig. 3). There was no hypotensive effect of RD in BPN/3J mice at 3 weeks compared to baseline and this was shown both during the dark and light period (Fig. 3). Similarly, the maintenance of MAP over the 3-week period in sham mice of both strains was evident in both the light and dark (Fig. 4). By contrast, the HR gradually reduced over the 3-week period in BPH/2J.
Effect of RD on cardiovascular variability and cardiac baroreceptor sensitivity
During the dark (active) period, mid frequency and high frequency MAP and HR power were 2–3-fold greater in BPH/2J than in BPN/3J mice (Table 2, P < 0.05) but baroreflex gain were similar between strains (Table 2). Low frequency and total MAP and HR power were similar in the 2 strains (Table 2). RD had no effect on any frequency MAP or HR power in BPN/3J mice and MAP power in BPH/2J. However, all frequency of HR power was less in BPH/2J RD mice compared to sham (Table 2). Also there was a trend for baroreflex gain to be less in RD BPH/2J compared to sham (Table 2, P = 0.060).
During the inactive period, only MAP, HR and mid frequency HR power were higher in sham BPH/2J compared to sham BPN/3J. MAP power, other HR frequencies and baroreflex gain were similar between the 2 strains (Supplementary Table 1). RD reduced day (inactive) HR in BPN/3J but had no other effects on MAP power or HR power or baroreflex gain. RD reduced MAP in BPH/2J but did not affect other inactive power spectral parameters in this strain (Supplementary Table 1).
Effects of RD on cardiovascular responses to enalaprilat and pentolinium during the active and inactive period
The acute hypotensive effects of enalaprilat were small and only observed in BPH/2J during the active period and not in BPN/3J (−3.4 mmHg in BPH/2J vs +3.0 mmHg in BPN/3J, Pstrain = 0.04, Fig. 5). During the active (dark) period, treatment with the ACE inhibitor enalaprilat following RD in BPH/2J mice induced a greater reduction in MAP from baseline compared to the sham procedure (−11.6 ± 1.8 vs −3.4 ± 1.8 mmHg, respectively, PRD = 0.01, Fig. 5). Conversely, in BPN/3J mice, treatment with enalaprilat had no effect on MAP, regardless of whether it was after RD or sham surgery (Fig. 5). Injection of the ganglion blocker pentolinium after enalaprilat treatment caused a similar depressor response in RD and sham BPH/2J mice (−50 ± 3 and −45 ± 4 mmHg, respectively, Fig. 5) which was also similar in RD and sham BPN/3J mice (−35 ± 4 vs −28 ± 4 mmHg, respectively, PRD = 0.2, Fig. 5). The depressor response to pentolinium during the active period was greater in BPH/2J mice compared with BPN/3J mice, regardless of whether mice underwent sham or RD (Pstrain < 0.002).
Average mean arterial pressure (MAP) responses to enalaprilat a, b and pentolinium c, d administration after pre-treatment with enalaprilat during the dark active period (left panels) or light inactive period (right panels) 2 weeks after renal denervation (RD, filled symbol) or sham surgery (open symbol) in genetically hypertensive BPH/2J (squares) and normotensive BPN/3J mice (circles). Histograms are mean change ± SEM from control period in BPN/3J sham mice (Grey unfilled, n = 10–11) and BPN/3J RD (grey filled, n = 6–7), BPH/2J sham (black unfilled, n = 8), BPH RD (black filled, n = 10) and were analysed by split plot analysis of variance. A probability of P < 0.05 was considered significant. *P < 0.05, **P < 0.01 and ***P < 0.001 for comparison of sham treatment with RD
During the inactive (light) period, there was a marked difference in the effect of enalaprilat administration on MAP between the 2 groups of BPH/2J mice, with a fall in MAP after RD (−4.2 ± 2.9 mmHg) but a rise in MAP in sham treated mice (10 ± 2 mmHg, PRD = 0.004, Fig. 5). Conversely, in BPN/3J mice, enalaprilat had little effect on MAP after sham surgery or RD (Fig. 5). Pentolinium injection after enalaprilat induced similar marked depressor responses in both RD and sham BPH/2J mice and also similar in RD and sham BPN/3J mice (Fig. 5). The depressor response to pentolinium during the inactive period was greater in BPH/2J mice compared with BPN/3J mice, regardless of whether mice underwent sham or RD (Pstrain < 0.001).
Effects of RD on cardiovascular responses to cage-switch, feeding and restraint tests
RD decreased the hypertensive effect of dirty cage-switch in BPH/2J mice by 21 % (PRD < 0.001) but had no effect on the response in BPN/3J mice (Supplementary Figure 2). The tachycardia induced by cage-switch was reduced by RD in both BPH/2J and BPN/3J mice (PRD < 0.05). RD did not alter the elevated locomotor activity observed in BPH/2J mice but reduced it in BPN/3J mice (P = 0.014, Supplementary Figure 2).
RD did not affect the cardiovascular responses or locomotor activity during the feeding or the restraint test in either BPH/2J and BPN/3J mice (Supplementary Figures 3 and 4).
Effects of RD on plasma renin, intrarenal renin and intrarenal Ren1 mRNA levels
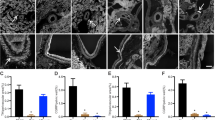
Intrarenal renin protein was similar in BPN/3J and BPH/2J but reduced in both strains by RD (P < 0.05 for both, Fig. 6). By contrast plasma renin levels were similar in both strains with intact or denervated renal nerves (Fig. 6). The expression of Ren1 mRNA was 1.6-fold higher in kidneys of sham BPH/2J mice compared to sham BPN/3J mice (Pstrain = 0.002, Fig. 6) and RD abolished the difference between strains (Fig. 6). The expression of PRR mRNA in sham-treated mice was ~ 30% lower in BPH (n = 8) compared with BPN mice (n = 8, P = 0.002, Fig. 6). There was no difference in PRR mRNA abundance in sham compared with renal denervated BPN/3J (n = 7, P = 0.74) or BPH/2J mice (n = 10, P = 0.16).
Bar graphs (top) show levels of Ren1 mRNA, Prorenin receptor (PRR) mRNA and (bottom) renal renin protein, plasma renin protein of normotensive BPN/3J sham mice (Unfilled white, n = 6–8) and BPN/3J renal denervated (RD) (white hatched, n = 5–7), BPH/2J sham (BPH, grey, n = 4–8), BPH RD (grey hatched, n = 5–12). Data are expressed as mean ± SEM and were analysed by split plot analysis of variance. A probability of P < 0.05 was considered significant. *P < 0.05 for comparison of sham treatment with RD; #P < 0.05, ##P < 0.01 and ###P < 0.001 for comparison of BPH/2J and BPN/3J mice
Effects of RD on renal noradrenaline levels
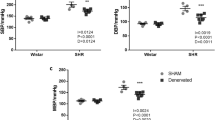
Renal noradrenaline content in the kidneys of sham denervated BPH/2J mice was 342 ± 16 pg/g being 1.7 times higher than the 200 ± 23 pg/g measured in sham denervated BPN/3J mice (Pstrain < 0.001). After RD, noradrenaline content was 112 ± 15 pg/g in BPH/2J mice compared to shams (PRD < 0.001) and 99 ± 15 pg/g in BPN/3J mice (PRD = 0.004). Thus, noradrenaline content of the kidney after RD was similar in both strains. In BPH/2J there tended to be a correlation between the level of noradrenaline in the kidney and the hypotensive effect of RD or sham treatment measured after 3 weeks (r = 0.56, n = 12, P = 0.056) but this was not evident in BPN/3J mice (Supplementary Figure 5).
Discussion
The present study shows that BPH/2J mice have elevated renal noradrenaline levels compared with BPN/3J mice, providing support for enhanced renal sympathetic activity in this hypertensive strain. Importantly, RD resulted in a 46% reduction in the hypertension over 3 weeks, whereas sham surgery had minimal effect on MAP in BPH/2J mice. By contrast, denervation had little effect on MAP in BPN/3J mice. Thus, our findings support an important role for renal nerves in the hypertension in BPH/2J mice. The reduction in MAP in denervated BPH/2J mice was not likely due to a reduction in the SNS vasomotor tone as the hypotension produced by pentolinium was the same in denervated and sham BPH/2J. Also, there was not a reduction in the tonic vasomotor effects of the RAS as evidenced by the rapid effect of ACE inhibitor enalaprilat (within 30 min). Indeed, the hypotensive effects of enalaprilat actually increased after RD in BPH/2J suggesting a partial compensatory mechanism rather than the reason for the MAP reduction. Interestingly, this occurred without any change to plasma renin protein levels. We found that there was higher renin mRNA level in the kidney of BPH/2J compared to normotensive BPN/3J. The antihypertensive effects produced by RD were associated with reductions in intrarenal renin protein levels accompanied by lower levels of renal renin mRNA compared to sham BPH/2J mice. Taken together, these findings support the notion that the integrity of renal nerves is important for maintaining hypertension in BPH/2J mice and that the antihypertensive effects of RD were associated with a reduction in renal renin mRNA. These findings are consistent with the proposal by Marques et al. of the important role of intrarenal renin in human hypertension [20].
The reduction in MAP produced by RD was similar during the active and inactive phase in BPH/2J suggesting that the effect is independent of activity (see Fig. 1). It is therefore similar to the pattern observed following MeAm lesions in this strain, which produced an 11 mmHg reduction in MAP during both the inactive and active phase [3]. However, the RAS and the SNS contributions were attenuated in the BPH/2J with lesions of the MeAm, which contrasts the current study. RD had also very little effect on the response to stress. In the present study, RD reduced the pressor response to dirty cage-switch stress in BPH/2J mice but did not affect the pressor response to other stressors. Thus, the hypotensive effect of RD is not a consequence of attenuated stress reactivity involving the SNS. Furthermore, we did not observe any significant reduction in the augmented locomotor activity associated with BPH/2J mice [19]. We also observed a reduction in HR but this was similar in both sham and RD mice and therefore, unrelated to RD. We have seen a similar reduction in HR in BPH/2J over 3 weeks in a previous study not involving RD [3]. Interestingly there was a reduction in baroreflex gain in BPH/2J, which was due to a reduction in the HR power (at all frequencies) rather than a change in fluctuations in MAP (see Table 2) and as such reflects less cardiac vagal activity. A small temporary reduction in body weight was observed in the RD mice, presumably due to loss of fluid related to increased urine production which is normally observed after RD [21]. Both body weight and activity were similar to baseline levels by the 3rd week following denervation or sham treatment and were not different between groups, suggesting a likely specific effect on the cardiovascular system of the RD.
The reduction in MAP of 8 mmHg which we observed after RD in BPH/2J mice was similar to that reported by Hart et al. in SHR 6–9 days after surgical RD and in human subjects 6 months after catheter-based RD [22]. Similar effects of RD have been shown in other models of hypertension including that induced by hyperinsulinemia [23], DOCA-salt hypertension [24], in offspring from rats with reduced uterine perfusion [25], in Dahl salt-sensitive [26], SHR [22, 27, 28] and in rats with induced cardio-renal syndrome [29]. Whereas some studies showed that RD fully abolished hypertension, demonstrating similar BP between hypertensive and normotensive models after RD [25, 30], Machino et al. reported a 20% reduction in systolic BP of SHR 3 months after radiofrequency RD without reaching a MAP comparable with normotensive rats [28]. These findings are in accordance with recent studies in humans, in which the blood pressure of hypertensive patients did not reach normal values following RD [31]. However, despite numerous denervation studies, few have elucidated the underlying mechanism. To assess the contribution of the SNS with and without RD, we applied ganglion blockade after ACE inhibition, as this reduces the compensatory response of the RAS to the fall in MAP, unmasking the full contribution of the SNS [4]. We assessed the contribution of the SNS and the RAS at the end of the experiment but the reduction in MAP we observed in BPH/2J was evident within 3 days and remained relatively stable over the 3-week period. Our observation that the depressor response to ganglion blockade with pentolinium was not altered by RD in BPH/2J mice, suggests that renal nerve ablation did not impact overall SNS-related vasomotor activity. This is surprising as we have removed sympathetic drive to the kidney suggesting that other beds may have compensated for the loss of renal vasomotor activity. Similarly, ganglion blockade after RD showed little difference to the response in BPN/3J mice. We have included spectral analysis in the present study as we have previously shown that the mid frequency power is greater in BPH/2J compared to BPN/3J and that this reflects the augmented sympathetic activity in the hypertensive strain [3]. In the present study we did not observe any difference between the RD and sham mice in this frequency which supports the findings with ganglionic blockade that SNS activity has not been affected by RD. The intact pressor response to restraint stress, which we have shown to be reliant on the SNS activation was well maintained suggesting that the activation of the SNS is not near maximal. Nevertheless, the effect of RD suggests that the enhanced SNS contribution is predominantly in extra-renal beds.
In the present study, renal catecholamine content was higher in BPH/2J mice than their normotensive counterparts, which may be an indicator of greater renal SNA in hypertensive mice and provides further support for renal sympathetic overactivity being closely associated with the hypertension. Renal noradrenaline content in SHR, stroke-prone SHR and diabetic rats was similarly elevated compared with normotensive controls [28, 32, 33]. The degree of reduction being 50–70% in the present study was more than what is achieved by radiofrequency lesions in rats or humans [28, 34], but not as complete as in some studies [35]. Other studies reported that RD decreased renal catecholamines in hypertensive rats to the levels observed in normotensive controls [28, 32, 33, 36]. Renal noradrenaline spillover was also markedly reduced after renal nerve ablation in humans [34]. However, as previously described in other animal models [25, 28, 37], we observed that RD also reduced renal noradrenaline in normotensive animals without affecting BP. We have previously observed a small fall in MAP in normotensive rabbits following RD in the order of 6 mmHg and also an enhanced depressor response to ganglionic blockade which is unlike the effects seen in the present study [38].
We have previously reported greater renal sympathetic innervation in BPH/2J mice as well as enhanced Ren1 mRNA in the kidney, which may be mechanistically associated [4]. In the present study, we found a small but significantly greater response to ACE inhibitor enalaprilat in sham BPH/2J compared with BPN/3J mice, confirming previous findings [4] which suggest a greater contribution of the RAS to BP maintenance in BPH/2J mice. In sham BPH/2J mice, expression of renal renin mRNA was greater, whereas PRR mRNA was lower than sham BPN/3J mice but there was no difference in plasma renin nor renal protein levels between strains in the sham groups. Although we found that renal renin protein was lower in the denervated groups than sham for both BPN and BPH mice, it is important to note that renin protein in the kidney closely reflects renin storage level, whereas, Ren1 mRNA, which was only lower in denervated BPH/2J but not BPN/3J mice, is more stimulus dependent and thus reflective of the state of renin production [39]. In this study, mRNA levels may be more informative since we are measuring the effect of SNA, which dynamically influences renin expression. Since renal denervation only decreases renal renin protein but not mRNA in BPN mice, it is possible that while denervation has decreased renin stores in BPN mice, they have maintained adequate renin production to maintain BP. Furthermore, given BPH/2J mice seem to have a far greater dependence on RSNA to maintain BP, it is possible that BPN mice are more able to compensate for the loss of RSNA with other regulatory mechanisms. In the present study RD had no effect on either renal PRR or plasma renin protein levels in either strain. However, we have not measured renin enzyme activity, thus it is possible that plasma renin enzyme activity may be elevated in sham BPH and may be lowered following denervation. Indeed, RD has been shown to reduce plasma renin activity in SHR [28].
In conclusion, we suggest that hypertension in BPH/2J mice involves overactivity of predominantly the SNS but also higher activity intrarenal RAS in the kidney and it is the latter mechanism, which is responsible for the long-term antihypertensive effects of RD. These findings support the continued use of RD in the treatment of hypertension in humans and explain the mechanisms involved.
References
Schlager G. Selection for blood pressure levels in mice. Genetics. 1974;76:537–49.
Davern PJ, Nguyen-Huu T, La Greca L, Head GA. Role of the sympathetic nervous system in Schlager genetically hypertensive mice. Hypertension. 2009;54:852–9.
Jackson KL, Palma-Rigo K, Nguyen-Huu T-P, Davern PJ, Head GA. Major contribution of the medial amygdala to hypertension in BPH/2J genetically hypertensive mice. Hypertension. 2014;63:811–8.
Jackson KL, Marques FZ, Watson AMD, Palma Rigo K, Nguyen-Huu T-P, Morris BJ, et al. A novel interaction between sympathetic overactivity and aberrant regulation of renin by mir-181a in BPH/2J genetically hypertensive mice. Hypertension. 2013;62:775–81.
Liard JF. Renal denervation delays blood pressure increase in the spontaneously hypertensive rat. Experientia. 1977;33:339–40.
Jacob F, Clark LA, Guzman PA, Osborn JW. Role of renal nerves in development of hypertension in DOCA-salt model in rats: a telemetric approach. Am J Physiol Heart Circ Physiol. 2005;289:H1519–29.
Osborn JL, Roman RJ, Ewens JD. Renal nerves and the development of Dahl salt-sensitive hypertension. Hypertension. 1988;11(6 Pt 1):523–8.
Kandlikar SS, Fink GD. Mild DOCA-salt hypertension: sympathetic system and role of renal nerves. Am J Physiol Heart Circ Physiol. 2011;300:H1781–87.
Moretti J-L, Burke SL, Evans RG, Lambert GW, Head GA. Enhanced responses to ganglion blockade do not reflect sympathetic nervous system contribution to Angiotensin II-induced hypertension. J Hypertens. 2009;27:1838–48.
Esler M. The sympathetic nervous system in hypertension: back to the future? Curr Hypertens Rep. 2015;17:519.
Krum H, Schlaich MP, Sobotka PA, Bohm M, Mahfoud F, Rocha-Singh K, et al. Percutaneous renal denervation in patients with treatment-resistant hypertension: final 3-year report of the Symplicity HTN-1 study. Lancet. 2014;383:622–9.
Townsend RR, Mahfoud F, Kandzari DE, Kario K, Pocock S, Weber MA, et al. Catheter-based renal denervation in patients with uncontrolled hypertension in the absence of antihypertensive medications (SPYRAL HTN-OFF MED): a randomised, sham-controlled, proof-of-concept trial. Lancet. 2017;390:2160–70.
Butz GM, Davisson RL. Long-term telemetric measurement of cardiovascular parameters in awake mice: a physiological genomics tool. Physiol Genom. 2001;5:89–97.
Wang W, Falk SA, Jittikanont S, Gengaro PE, Edelstein CL, Schrier RW. Protective effect of renal denervation on normotensive endotoxemia-induced acute renal failure in mice. Am J Physiol Ren Physiol. 2002;283:F583–87.
Jackson KL, Head GA, Morris BJ, Chin-Dusting J, Jones E, La Greca L, et al. Reduced cardiovascular reactivity to stress but not feeding in renin enhancer knockout mice. Am J Hypertens. 2007;20:893–9.
Lee DL, Webb RC, Brands MW. Sympathetic and angiotensin-dependent hypertension during cage-switch stress in mice. Am J Physiol Regul Integr Comp Physiol. 2004;287:R1394–98.
Lambert GW, Jonsdottir IH. Influence of voluntary exercise on hypothalamic norepinephrine. J Appl Physiol. 1998;85:962–6.
Ludbrook J. Repeated measurements and multiple comparisons in cardiovascular research. Cardiovasc Res. 1994;28:303–11.
Jackson KL, Nguyen-Huu T-P, Davern PJ, Head GA. Energy metabolism in BPH/2J genetically hypertensive mice. Hypertens Res. 2014;37:413–21.
Marques FZ, Romaine SP, Denniff M, Eales J, Dormer J, Garrelds IM, et al. Signatures of miR-181a on renal transcriptome and blood pressure. Mol Med. 2015;21:739–48.
Bello-Reuss E, Colindres RE, Pastoriza-Munoz E, Mueller RA, Gottschalk CW. Effects of acute unilateral renal denervation in the rat. J Clin Investig. 1975;56:208–17.
Hart EC, McBryde FD, Burchell AE, Ratcliffe LE, Stewart LQ, Baumbach A, et al. Translational examination of changes in baroreflex function after renal denervation in hypertensive rats and humans. Hypertension. 2013;62:533–41.
Huang WC, Fang TC, Cheng JT. Renal denervation prevents and reverses hyperinsulinemia-induced hypertension in rats. Hypertension. 1998;32:249–54.
Katholi RE, Naftilan AJ, Oparil S. Importance of renal sympathetic tone in the development of DOCA-salt hypertension in the rat. Hypertension. 1980;2:266–73.
Alexander BT, Hendon AE, Ferril G, Dwyer TM. Renal denervation abolishes hypertension in low-birth-weight offspring from pregnant rats with reduced uterine perfusion. Hypertension. 2005;45:754–8.
Foss JD, Fink GD, Osborn JW. Differential role of afferent and efferent renal nerves in the maintenance of early- and late-phase Dahl S hypertension. Am J Physiol Regul Integr Comp Physiol. 2016;310:R262–67.
Foss JD, Fink GD, Osborn JW. Reversal of genetic salt-sensitive hypertension by targeted sympathetic ablation. Hypertension. 2013;61:806–11.
Machino T, Murakoshi N, Sato A, Xu D, Hoshi T, Kimura T, et al. Anti-hypertensive effect of radiofrequency renal denervation in spontaneously hypertensive rats. Life Sci. 2014;110:86–92.
Eriguchi M, Tsuruya K, Haruyama N, Yamada S, Tanaka S, Suehiro T, et al. Renal denervation has blood pressure-independent protective effects on kidney and heart in a rat model of chronic kidney disease. Kidney Int. 2015;87:116–27.
Winternitz SR, Katholi RE, Oparil S. Decrease in hypothalamic norepinephrine content following renal denervation in the one-kidney, one clip Goldblatt hypertensive rat. Hypertension. 1982;4:369–73.
Esler MD, Krum H, Sobotka PA, Schlaich MP, Schmieder RE, Bohm M. Renal sympathetic denervation in patients with treatment-resistant hypertension (The Symplicity HTN-2 Trial): a randomised controlled trial. Lancet. 2010;376:1903–9.
Wang T, Nabika T, Notsu Y, Takabatake T. Sympathetic regulation of the renal functions in rats reciprocally congenic for chromosome 1 blood pressure quantitative trait locus. Hypertens Res. 2008;31:561–8.
Yao Y, Fomison-Nurse IC, Harrison JC, Walker RJ, Davis G, Sammut IA. Chronic bilateral renal denervation attenuates renal injury in a transgenic rat model of diabetic nephropathy. Am J Physiol Ren Physiol. 2014;307:F251–62.
Krum H, Schlaich M, Whitbourn R, Sobotka PA, Sadowski J, Bartus K, et al. Catheter-based renal sympathetic denervation for resistant hypertension: a multicentre safety and proof-of-principle cohort study. Lancet. 2009;373:1275–81.
Kim J, Padanilam BJ. Renal nerves drive interstitial fibrogenesis in obstructive nephropathy. J Am Soc Nephrol. 2013;24:229–42.
Bao G, Metreveli N, Li R, Taylor A, Fletcher EC. Blood pressure response to chronic episodic hypoxia: role of the sympathetic nervous system. J Appl Physiol. 1997;83:95–101.
Franquini JV, Medeiros AR, Andrade TU, Araujo MT, Moyses MR, Abreu GR, et al. Influence of renal denervation on blood pressure, sodium and water excretion in acute total obstructive apnea in rats. Braz J Med Biol Res. 2009;42:214–9.
Burke SL, Evans RG, Moretti J-L, Head GA. Levels of renal and extrarenal sympathetic drive in Ang II-induced hypertension. Hypertension. 2008;51:878–83.
Markus MA, Goy C, Adams DJ, Lovicu FJ, Morris BJ. Renin enhancer is crucial for full response in Renin expression to an in vivo stimulus. Hypertension. 2007;50:933–8.
Acknowledgements
We acknowledge the technical assistance of Thu-Phuc Nguyen-Huu and John-Luis Moretti.
Funding
This work was supported by grants from the National Health & Medical Research Council of Australia (NHMRC, Project grant 1065714) and in part by the Victorian Government’s OIS Program. Investigators were supported by NHMRC/NHF Postdoctoral Fellowships (APP1012881 to P.J.D. NHMRC APP1052659 and National Heart Foundation PF12M6785/101185 co-shared to F.Z.M., NHMRC APP1091688 to K.L.J.) and NHMRC Research Fellowships to G.W.L.: APP1042492 and G.A.H.: APP1002186).
Author contributions
C.G., K.L.J., F.Z.M., N.E., S.P., and E.R.S. performed the study including experimental data collection, assays and analysis. C.G., K.L.J., F.Z.M., N.E., S.P., E.R.S., F.J.C., G.W.L., P.J.D., and G.A.H. contributed to the analysis, writing and preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
G.W.L. received research support from Medtronic and has acted as a consultant for Medtronic.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Gueguen, C., Jackson, K.L., Marques, F.Z. et al. Renal nerves contribute to hypertension in Schlager BPH/2J mice. Hypertens Res 42, 306–318 (2019). https://doi.org/10.1038/s41440-018-0147-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-018-0147-9
Keywords
This article is cited by
-
Cardiorenal syndrome: long road between kidney and heart
Heart Failure Reviews (2022)
-
Effect of renal denervation on long-term outcomes in patients with resistant hypertension
Cardiovascular Diabetology (2021)
-
Renal denervation does not affect hypertension or the renin-angiotensin system in a rodent model of juvenile-onset polycystic kidney disease: clinical implications
Scientific Reports (2021)
-
Neural suppression of miRNA-181a in the kidney elevates renin expression and exacerbates hypertension in Schlager mice
Hypertension Research (2020)
-
Mechanisms underlying the effects of renal denervation in renovascular hypertension
Hypertension Research (2019)