Abstract
HIV latency is the main barrier to HIV eradication. Peripheral T follicular helper (pTfh) cells have a prominent role in HIV persistence. Herein, we analyzed the HIV reservoir size within memory CD4+ T-cell subsets in patients with HIV replication control. Twenty HIV-infected patients with suppressed HIV replication were included, with 10 elite controllers (EC) and 10 treated (TX) individuals. The HIV reservoir size was analyzed in resting memory CD4+ T-cells (Trm), pTfh, and non-pTfh cells using an ultrasensitive digital-droplet-PCR assay. Inter-group and intra-group differences were tested using non-parametric tests. Compared with the TX patients, the EC patients had smaller HIV reservoir not only in Trm but also in pTfh and non-pTfh subsets of memory CD4+ T-cells. The largest differences were observed in pTfh cells (p = 0.025). The pTfh and non-pTfh cells harbored similar levels of HIV-DNA in the EC (p = 0.60) and TX patients (p = 0.17); however, the contribution to HIV-DNA levels in memory CD4+ T-cells varied among the pTfh and non-pTfh subsets in both groups of patients. The EC patients showed smaller HIV reservoir in memory CD4+ cells, especially in the pTfh subset, a population of cells with a pivotal role in the antiviral immune response, suggesting a potential link between low levels of infection in pTfh cells and the ability of the EC patients to spontaneously control HIV replication.
Similar content being viewed by others
Introduction
The HIV latent reservoir is the main barrier to HIV eradication. Although combination antiretroviral therapy (cART) can effectively block viral replication in the host and reduce the circulating virus to undetectable levels1, antiviral therapy cannot completely eliminate the virus from the human body. As a result, the viral load rapidly rebounds within 2 to 8 weeks after cART discontinuation2,3,4. The rebound occurs due to the presence of anatomic reservoirs that drugs cannot easily access5. Additionally, there are reservoirs containing cells with HIV integrated into the cell genome. However, the viral genome is transcriptionally silent, and the virus is refractory to both cART and the immune system6,7,8.
The cellular reservoir may include several cell subpopulations, and the latent and long-term persistent virus has been described in resting memory CD4+ T-cells (Trm cells)9. This CD4+ T-cell subset with memory phenotype (CD45RO+) and low expression of activation markers such as HLA-DR, CD25 or CD699 allow the establishment of latent reservoir extremely stable with a mean half-life of around 44 months10,11. There is another memory CD4+ T-cell subpopulation present in germinal centers, T follicular helper (Tfh) cells. Tfh cells have a prominent role in regulating the HIV reservoir by supporting persistent infection, replication, and production of HIV in both viremic HIV-infected subjects12 and long-term cART-treated aviremic individuals13. Tfh cells are a memory CD4+ T-cell subset expressing CXCR5 and have B cell helper function localized within secondary lymphoid organs14. The counterpart in peripheral blood is called the peripheral Tfh (pTfh) cells because they display functional properties similar to Tfh cells and represent approximately 20% of total memory CD4 T-cells15,16,17. Although several markers have been associated to pTfh cells (CXCR5, CXC3, CCR7, PD1)15,17,18,19,20,21,22,23, only the expression of CXC chemokine receptor 5 (CXCR5) has been considered as a specific marker for total pTfh cells15. Some differences between pTfh and Tfh cells regarding expression of surface markers have been noticed, such as the low expression of PD-1 in pTfh cells17 in contrast to the high expression of this marker by Tfh cells24,25,26, suggesting that pTfh cells would be in a resting state similar to Trm cells17.
Accessing the lymph nodes of HIV-infected patients is a complex and invasive procedure. Thus, the availability of pTfh cells in blood represents an important step for the understanding of HIV infection and persistence in this compartment. Several studies have focused on the role of pTfh cells in HIV infection18,19,20. However, only one recent study has focused in the role of pTfh cells in HIV persistence in patients before and after the initiation of cART22.
Elite controller (EC) patients are a model for the development of therapeutic strategies aimed at functional HIV cure27. There is extensive literature on the ability of these subjects to spontaneously maintain HIV replication control27,28. A few recent studies evaluated their ability to maintain better control of the HIV reservoir size29,30,31. However, these studies mostly used peripheral blood mononuclear cells (PBMCs)29,30 and resting CD4+ T-cell subsets31. There are no studies examining pTfh cells, which have a prominent role in HIV reservoir. Therefore, we have characterized the reservoir size in different memory CD4+ T-cell subpopulations. We examined the Trm cells, pTfh cells, and non-pTfh cells from EC patients and compared the results with those from treatment-controlled HIV-patients (TX, aviremic patients with cART).
Results
Baseline characteristics of the study population
The EC and TX patient groups were comparable with respect to age, gender, CD4 counts, and length of infection (Table 1). The median follow-up of EC patients maintaining EC status was 7 [3–12] years, and 7 of 10 subjects had more than 5 years of EC status. During the follow-up period, all EC patients showed high and stable CD4 counts (897 [771–1,187] at the beginning and 912 [630–1,438] cells/µL at the end of follow-up, p = 0.86).
EC patients have a smaller HIV reservoir than do TX patients
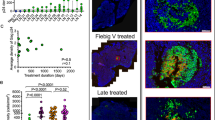
We found lower levels of HIV-DNA in Trm cells in the EC group than in those in the TX group (median [IQR]: 381 [74–1,002] vs. 1197 [619–1,623] copies/million cells respectively; p = 0.059), showing that EC maintain a lower HIV reservoir in this cell population than do patients with cART-mediated long-term suppression of HIV replication (Fig. 1a). Furthermore, we found the HIV reservoir size in pTfh cells was significantly lower in patients able to spontaneously control HIV replication (88 [33–291] copies/million cells) than that in patients with cART-mediated viral suppression (723 [393–1,199] copies/million cells; p = 0.025) (Fig. 1a). Interestingly, this difference between EC and TX patients was less pronounced in non-pTfh cells (162 [18–1,871] vs. 989 [600–1,354]) and was not significant (p = 0.172) (Fig. 1a).
Box-plot graphs showing: (a) HIV reservoir size (HIV-DNA copies per million of cells) in Trm, pTfh and non-pTfh cells of the HIV-infected groups with suppressed HIV replication (EC and TX patients). (b) Percentage of Trm, pTfh and non-pTfh cells over the total CD4+ T-cells in HIV-infected groups with suppressed HIV replication (EC and TX patients). P-values of comparisons between the EC and TX groups of patients by Mann-Whitney U-test, and between pTfh and non-pTfh cell subsets by Wilcoxon signed- rank test are shown.
HIV reservoir size is not influenced by frequency of the different analyzed CD4+ T-cell subsets
We evaluated the possibility that HIV reservoir size in EC or TX patients may be influenced by the relative frequency of specific CD4+ T-cell populations. Therefore, we assessed the frequencies of each T-cell subset involved in maintaining the HIV reservoir (Trm, pTfh, and non-pTfh) for both groups of studied patients. The frequencies of Trm, pTfh, and non-pTfh cells were similar for both groups of studied patients (Fig. 1b). We next evaluated the correlation between the size of HIV reservoir in the different CD4+ T-cell subsets and their frequency in EC and TX subjects. There was no correlation between HIV-DNA levels in Trm and the frequency of Trm within the total CD4+ T-cells (Spearman’s rho = 0.02; p = 0.93). Additionally, there was no relationship between HIV-DNA levels in pTfh and the frequency of pTfh in the total CD4+-T-cell population (Spearman’s rho = −0.15; p = 0.56). Similar results were observed in non-pTfh cells (Spearman’s rho = 0.27; p = 0.30).
pTfh and non-pTfh cell subsets contribute to HIV reservoir size
We confirmed the contribution of the Trm cell subset to HIV reservoir size. The Trm cells represent a specific cell subset among memory CD4+ T-cells. We found no statistically significant differences in levels of HIV-DNA (copies/million cells) between pTfh and non-pTfh cells in both EC (pTfh: 88 [33–291] vs non-pTfh: 162 [18–1,871]; p = 0.600) and TX (pTfh: 723 [393–1,199] vs non-pTfh: 989 [600–1,354]; p = 0.169) patients (Fig. 1a). This finding suggests both subsets contribute to HIV persistence. However, among total memory CD4+ T-cells (comprising pTfh and non-pTfh cell subsets) the proportion of non-pTfh was higher than the proportion of pTfh cells in both EC patients (70% [66–78] vs 30% [22–35] respectively; p = 0.018) and TX patients (76% [68–78] vs 24% [22–32] respectively; p = 0.005) (Fig. 1b). Therefore, the relative contribution to the HIV reservoir size in total memory CD4+ T-cells was higher for the non-pTfh cells than the pTfh cells in both EC and TX patients (Fig. 2).
Discussion
To our knowledge, this is the first study analyzing the levels and relative contribution of HIV-DNA from Trm, pTfh, and non-pTfh subsets of memory CD4+ T-cells to the HIV reservoir size in both patients with long-term spontaneous control of HIV replication (EC) and in patients with cART-mediated long-term suppression of HIV replication (TX). In this study, compared with TX patients, EC patients showed a smaller HIV reservoir. This finding is in agreement with a previous report analyzing levels of HIV-DNA in resting central memory CD4+ T-cells from elite controller patients31.
Tfh cells and their counterpart in peripheral blood (pTfh cells) have recently become a key aspect of HIV infection18,19,20,21,32,33 and the persistent reservoir12,13,22. Compared with other subsets of memory CD4+ cells, the Tfh cells located in the lymph nodes of progressing HIV-infected patients harbored higher levels of replication-competent HIV-DNA12,13. A recent study found similar results using pTfh cells from progressor patients before and after cART22. Interestingly, we found that the HIV reservoir size in pTfh was smaller in patients able to spontaneously control HIV replication than that in patients with cART-mediated viral suppression. This result suggests that host-mediated containment of HIV replication observed in EC patients might reduce the HIV reservoir, especially in the pTfh cell population compared with other memory CD4+ T-cell populations such as non-pTfh cells. Moreover, pTfh cells can support the HIV-specific cellular response16 and HIV-specific broadly neutralizing antibody production in HIV-infected typical progressing patients17 and in EC subjects23. Thus, the low level of HIV infection in pTfh cells from EC patients could help to preserve their functionality and impacts the ability of EC patients to maintain control of HIV replication.
It is also important to note that the study by Perreau et al. found that Tfh cells are expanded in HIV-infected subjects and decreased after cART12. Therefore, the lower total HIV-DNA that we observed in pTfh of EC patients could be due to a “dilution effect” as a consequence of a higher frequency of pTfh cells in EC. However, our results show that was not the case since frequency of pTfh cells was similar for both EC and TX patients, and there was no correlation between reservoir size in the pTfh cell subset and their relative frequency within CD4+ T-cells.
Moreover, HIV infection is controlled early in EC patients34,35. This finding may provide insight into the mechanism explaining the lower HIV reservoir size observed in EC patients compared with that in TX patients in whom cART-induced HIV replication control occurs later since they usually start therapy at least one year after infection. Moreover, since pTfh cells are more supportive for HIV replication22 the lower levels of HIV-DNA that we also found in the Trm cells of EC patients could be the consequence of the lower amount of pTfh cells harboring HIV-DNA observed in these patients.
There are several controversial issues in our study. First, the definition of the pTfh cell subset is variable in the literature and this is problematic because it is difficult to compare and interpret results from different studies. Several markers (CXCR5, CXC3, CCR7, PD1) have been associated with pTfh cells15,17,18,19,20,21,22,23. However, the majority of the markers are not pTfh cell-specific and CXCR3, CCR7 or PD1 have been used in studies to distinguish different pTfh functional states and have found controversial results17,22,23. Currently, the most definitive/unambiguous marker available to identify both Tfh36,37 and circulating Tfh (pTfh)15,18,21,22,38 cells is the expression of CXC chemokine receptor 5 (CXCR5), which includes the distinct pTfh subsets with different capacities to regulate B cell responses. Second, a previous study suggests that EC patients have an excess of unintegrated HIV DNA30; thus, the measurement of total HIV-DNA and the absence of virus growth assays to evaluate replication-competent virus in our study could interfere with our data analysis; however, several authors recently noted the relevance of measuring total HIV-DNA as a marker of viral reservoir dynamics with clinical implications39,40. The authors suggested that both integrated and total HIV-DNA provides an inducible and functional reservoir and predicts ex vivo viral outgrowth40,41. Additionally, it has been highlighted that the establishment of HIV latency and virus production from unintegrated genomes follows direct infection of resting CD4+ T-cells42. Third, given the relevance of Tfh and pTfh cells in HIV reservoir maintenance12,13,22, our finding regarding no appreciable intragroup difference between pTfh cells and non-pTfh cells in HIV-DNA content could sounds controversial. However, since we could not measure replication-competent provirus we cannot rule out the possibility that pTfh may represent a major reservoir as compared to non-pTfh cells in HAART-treated patients, as it has been suggested by Pallikuth et al.22, and even in EC patients. Finally, a recent study reported that CD32a (the type II receptor for Fc fragment of IgG) is a cell surface marker specific for resting CD4+ T-cells carrying replication-competent HIV43. Thus, it will be essential to analyze the expression levels of this marker on the different CD4+ T-cell subsets contributing to HIV reservoir in future studies. It will also be valuable to determine the relationship between CD32a expression and HIV-DNA content in these cell subsets.
In summary, our study results show that elite controller patients maintain low levels of HIV-DNA in the pTfh cell subset, which is a population of memory CD4+ T-cells with special relevance in the maintenance of HIV persistence and in the generation of a robust virus-specific immune response. Our results also highlight the importance of monitoring HIV-DNA in different subsets of memory CD4+ T-cells, given their differential relevance in the phenomenon of viral persistence and their differential contribution to the extent of the HIV reservoir in peripheral blood. These findings may also have clinical relevance in future clinical trials aimed at purging the HIV reservoir, and studies with a larger cohort of patients could support our results.
Methods
Study population
This cross-sectional study was conducted in the following groups of chronically HIV-infected patients with suppressed HIV replication: 10 EC with undetectable plasma HIV-RNA (<50 copies/mL) without cART and 10 TX with at least five years of cART and complete viral suppression. The groups were matched for age, sex, length of infection and CD4+ T-cell counts. An HIV-infected patient was considered an EC when having at least three consecutive plasma HIV viral load determinations with no more than 50 HIV-RNA copies/mL during at least 12 months of follow-up in absence of any combination of antiretroviral therapy (cART). The EC patients included in our study had long-term control of HIV replication and stable CD4 counts during the whole follow-up period. The patients were recruited at different HIV-reference hospitals in Madrid, Spain. The recruitment period was 12 months. We started with the entire HIV population of each hospital, and the patients meeting the inclusion criteria and willing to participate in the study were selected. The study protocol was evaluated and approved by the Ethical review board of Instituto de Investigación Sanitaria-Fundación Jiménez Díaz, Madrid, Spain in accordance with the declaration of Helsinki. Each participating patient signed an informed consent form.
Cell samples
We collected two 300 mL EDTA-anticoagulated blood samples (6 months apart) from each participant to purify the different memory CD4+ T cell populations (Trm, pTfh and non-pTfh cells). One sample was used to isolate Trm cells and the other sample was used to isolate pTfh and non-pTfh cells. All the analyses were conducted using fresh peripheral blood mononuclear cells (PBMCs) isolated by density gradient centrifugation with Ficoll-Hypaque (Sigma Chemical Co., USA).
Immuno-magnetic purification of Trm, pTfh and non-pTfh cells
We isolated the following different CD4+ T-cell populations from total fresh PBMCs (without any stimulation to avoid the triggering of TCR): Trm (defined as CD4+CD45RO+CD25−CD69−HLADR−), pTfh (defined as CD4+CD45RO+CXCR5+), and non-pTfh (defined as CD4+CD45RO+CXCR5−). The cells were isolated using an immuno-magnetic separation technique (MACS microbeads system, Miltenyi Biotec, Madrid, Spain). The purification of each one of these cell subsets was preceded by a negative magnetic isolation of memory CD4+ T-cell subset (memory CD4 T-cell Isolation Kit) according to the manufacturer’s instructions. Trm cells were isolated through negative selection with a cocktail of monoclonal antibodies against CD25, CD69, and HLA-DR. pTfh cells were purified through positive selection using monoclonal antibody against CXCR5 (Clon REA103, Miltenyi Biotec). The non-labeled cells were collected since they included the non-pTfh cells. The purity of each isolated CD4+ memory cell subset was assessed by flow cytometry (SP6800 Spectral Analyzer, Sony, USA) and the purity was greater than 90% in all samples. A flow cytometry experiment illustrating the gating strategies for Trm, pTfh and non-pTfh cell subsets, as well as the purity after isolation of each cell subset is shown in Fig. 3.
Representative flow cytometry example of immuno-magnetic purification of Trm cells (a) and of pTfh and non-pTfh cells (b) before and after purification. The gating strategy and percentages of different T-cell populations are shown. Trm cells were defined as CD4+CD45RO+CD69−CD25−HLADR− cells. pTfh cells were defined as CD4+CD45RO+CXCR5+ cells and non-pTfh cells were defined as CD4+CD45RO+CXCR5− cells.
Cell-associated HIV-DNA quantification
Total DNA from purified Trm, pTfh, and non-pTfh cells of each patient was extracted using QIAamp DNA-MiniKit (Qiagen, USA) following the manufacturer’s instructions. The size of the proviral DNA reservoir of each cell subpopulation was measured as intracellular HIV-1 DNA copies per million cells using ultrasensitive digital-droplet PCR (ddPCR) as previously described44. DdPCR is a technique that measures total HIV-DNA as a marker of the HIV reservoir39,40 and has greater precision and reproducibility in the context of a low level of detection (as is the case of EC patients) compared with techniques that measure integrated HIV-DNA45. The contributions of the pTfh and non-pTfh subsets to the HIV reservoir in total memory CD4+ T-cells were calculated by accounting for the level of HIV-DNA in each of these subsets and their proportion among total memory CD4+ T-cells.
Statistical analysis
The main characteristics of the study groups are expressed as median [interquartile range]. Non-parametric Wilcoxon signed-rank test was used to evaluate differences between cell subpopulations among each group of patients, and Mann-Whitney U-test was used to evaluate the differences between patient groups in each cell subpopulation. All statistical analyses were performed using SPSS software version 15 (SPSS Inc., Chicago, IL, USA). All p-values were two-tailed and were considered significant only when lower than 0.05.
Data availability statement
All data generated or analyzed during this study are included in this published article.
References
Perelson, A. S. et al. Decay characteristics of HIV-1-infected compartments during combination therapy. Nature 387, 188–91 (1997).
de Jong, M. D. et al. Overshoot of HIV-1 viraemia after early discontinuation of antiretroviral treatment. AIDS 11, 79–84 (1997).
Chun, T. W., Davey, R. T. Jr., Engel, D., Lane, H. C. & Fauci, A. S. Re-emergence of HIV after stopping therapy. Nature 401(6756), 874–75 (1999).
Calin, R. et al. Treatment interruption in chronically HIV-infected patients with an ultralow HIV reservoir. AIDS 30(5), 761–69 (2016).
Lorenzo-Redondo, R. et al. Persistent HIV-1 replication maintains the tissue reservoir during therapy. Nature 530(7588), 51–56 (2016).
Chun, T. W. et al. Presence of an inducible HIV-1 latent reservoir during highly active antiretroviral therapy. Proc Natl Acad Sci USA 94, 13193–97 (1997).
Wong, J. K. et al. Recovery of replication-competent HIV despite prolonged suppression of plasma viremia. Science 278, 1291–95 (1997).
Finzi, D. et al. Identification of a reservoir for HIV-1 in patients on highly active antiretroviral therapy. Science 278, 1295–300 (1997).
Soriano-Sarabia, N. et al. Quantitation of replication-competent HIV-1 in populations of resting CD4+ T-cells. J Virol 88(24), 14070–77 (2014).
Finzi, D. et al. Latent infection of CD4+ T cells provides a mechanism for lifelong persistence of HIV-1, even in patients on effective combination therapy. Nat Med 5, 512–17 (1999).
Siliciano, J. D. et al. Long-term follow-up studies confirm the stability of the latent reservoir for HIV-1 in resting CD4+ T cells. Nat Med 9, 727–28 (2003).
Perreau, M. et al. Follicular helper T-cells serve as the major CD4 T-cell compartment for HIV-1 infection, replication, and production. J Exp Med 210(1), 143–56 (2013).
Banga, R. et al. PD-1(+) and follicular helper T-cells are responsible for persistent HIV-1 transcription in treated aviremic individuals. Nat Med 22(7), 754–61 (2016).
Kim, C. H. et al. Subspecialization of CXCR5+ T-cells: B helper activity is focused in a germinal center-localized subset of CXCR5+ T-cells. J Exp Med 193(12), 1373–81 (2001).
Morita, R. et al. Human blood CXCR5(+)CD4(+) T-cells are counterparts of T follicular cells and contain specific subsets that differentially support antibody secretion. Immunity 34(1), 108–21 (2011).
Schultz, B. T. et al. Circulating HIV-Specific Interleukin-21(+)CD4(+) T-cells Represent Peripheral Tfh Cells with Antigen-Dependent Helper Functions. Immunity 44(1), 167–78 (2016).
Locci, M. et al. Human circulating PD-1+CXCR3-CXCR5+ memory Tfh cells are highly functional and correlate with broadly neutralizing HIV antibody responses. Immunity 39(4), 758–69 (2013).
Boswell, K. L. et al. Loss of circulating CD4 T-cells with B cell helper function during chronic HIV infection. PLoS Pathog 10(1), e1003853 (2014).
Cubas, R. et al. Reversible Reprogramming of Circulating Memory T Follicular Helper Cell Function during Chronic HIV Infection. J Immunol 195(12), 5625–36 (2015).
Nicholas, K. J., Flaherty, D. K., Smith, R. M., Sather, D. N. & Kalams, S. A. Chronic HIV-1 infection impairs superantigen-induced activation of peripheral CD4+CXCR5+PD-1+ cells, with relative preservation of recall antigen-specific responses. J Acquir Immune Defic Syndr 74(1), 72–80 (2016).
Muir, R. et al. Altered Memory Circulating T Follicular Helper-B Cell Interaction in Early Acute HIV Infection. PLoS Pathog 12(7), e1005777 (2016).
Pallikkuth, S. et al. Peripheral T Follicular Helper Cells Are the Major HIV Reservoir within Central Memory CD4 T-cells in Peripheral Blood from Chronically HIV-Infected Individuals on Combination Antiretroviral Therapy. J Virol 90(6), 2718–28 (2015).
Martin-Gayo, E. et al. Circulating CXCR5+CXCR3+PD-1lo Tfh-like cells in HIV-1 controllers with neutralizing antibody breadth. JCI Insight 2(2), e89574 (2017).
Haynes, N. M. et al. Role of CXCR5 and CCR7 in follicular Th cell positioning and appearance of a programmed cell death gene-1high germinal center-associated subpopulation. J Immunol 179(8), 5099–108 (2007).
Nurieva, R. I. et al. Generation of T follicular helper cells is mediated by interleukin-21 but independent of T helper 1, 2, or 17 cell lineages. Immunity 29(1), 138–49 (2008).
Ma, C. S. et al. Early commitment of naïve human CD4(+) T cells to the T follicular helper (T(FH)) cell lineage is induced by IL-12. Immunol Cell Biol 87(8), 590–600 (2009).
Autran, B., Descours, B., Avettand-Fenoel, V. & Rouzioux, C. Elite controllers as a model of functional cure. Curr Opin HIV AIDS 6(3), 181–87 (2011).
Shasha, D. & Walker, B. D. Lessons to be Learned from Natural Control of HIV - Future Directions, Therapeutic, and Preventive Implications. Front Immunol 4, 162 (2013).
Julg, B. et al. Infrequent recovery of HIV from but robust exogenous infection of activated CD4 (+) T-cells in HIV elite controllers. Clin Infect Dis 51(2), 233–38 (2010).
Graf, E. H. et al. Elite suppressors harbor low levels of integrated HIV DNA and high levels of 2-LTR circular HIV DNA compared to HIV+ patients on and off HAART. PLoS Pathog 7(2), e1001300 (2011).
de Masson, A. et al. Blimp-1 overexpression is associated with low HIV-1 reservoir and transcription levels in central memory CD4+ T-cells from elite controllers. AIDS 28(11), 1567–77 (2014).
Pissani, F. & Streeck, H. Emerging concepts on TFH cell dynamics in HIV infection. Trends Immunol 35, 278–286 (2014).
Wang, X., Ziani, W. & Xu, H. Changes in follicular CD4+ T helper cells as a marker for evaluating disease progression in the competition between HIV and host immunity. Frontiers in Immunology 7, 474 (2016).
Okulicz, J. F. et al. Clinical outcomes of elite controllers, viremic controllers, and long-term nonprogressors in the US Department of Defense HIV natural history study. J Infect Dis 200(11), 1714–23 (2009).
Madec, Y., Boufassa, F., Porter, K. & Meyer, L. & CASCADE Collaboration. Spontaneous control of viral load and CD4 cell count progression among HIV-1 seroconverters. AIDS 19(17), 2001–7 (2005).
Schaerli, P. et al. CXC chemokine receptor 5 expression defines follicular homing T cells with B cell helper function. J Exp Med 192, 1553–62 (2000).
Breitfeld, D. et al. Follicular B helper T cells express CXC chemokine receptor 5, localize to B cell follicles, and support immunoglobulin production. J Exp Med 192, 1545–52 (2000).
Buranapraditkun, S. et al. Preservation of peripheral T follicular helper cell function in HIV controllers. J Virol [Epub ahead of print] (2017).
Avettand-Fènoël, V. et al. Total HIV-1 DNA, a Marker of Viral Reservoir Dynamics with Clinical Implications. Clin Microbiol Rev 29(4), 859–80 (2016).
Kiselinova, M. et al. Integrated and Total HIV-1 DNA Predict Ex Vivo Viral Outgrowth. PLoS Pathog 12(3), e1005472 (2016).
Petitjean, G. et al. Unintegrated HIV-1 provides an inducible and functional reservoir in untreated and highly active antiretroviral therapy-treated patients. Retrovirology 4, 60 (2007).
Chan, C. N. et al. HIV-1 latency and virus production from unintegrated genomes following direct infection of resting CD4 T cells. Retrovirology 13, 1 (2016).
Descours, B. et al. CD32a is a marker of a CD4 T-cell HIV reservoir harbouring replication-competent proviruses. Nature 543(7646), 564–7 (2017).
Strain, M. C. et al. Highly precise measurement of HIV DNA by droplet digital PCR. PLoS One 8(4), e55943 (2013).
Trypsteen, W., Kiselinova, M., Vandekerckhove, L. & De Spiegelaere, W. Diagnostic utility of droplet digital PCR for HIV reservoir quantification. J Virus Erad 2(3), 162–9 (2016).
Acknowledgements
We would like to thank all patients and healthy donors who participated in the study. This study has been funded by project CP14/00198 integrated in the State Plan for Scientific and Technical Research and Innovation and co-funded by ISCIII-Sub-Directorate General for Research Assessment and Promotion and European Regional Development Fund (ERDF). N Rallón is a Miguel Servet investigator from the Spanish Carlos III Institute of Health (ISCIII), grant CP14/00198, Madrid, Spain. M García is a predoctoral student co-funded by CP14/00198 project and the Intramural Research Scholarship from IIS-FJD.
Author information
Authors and Affiliations
Contributions
N.R. and J.M.B. conceived and designed the study. M.Go., M.F., A.C., J.C.L-B., F.J.D.L.H., V.E. and C.B. contributed to recruitment and follow-up of patients. M.Ga. and N.R. carried out the experimental work. M.M. and J.L. contributed to flow cytometry experiments. N.R., J.M.B. and M.Ga. performed the statistical analysis. N.R., J.M.B. and M.Ga. drafted the manuscript. All authors reviewed and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
García, M., Górgolas, M., Cabello, A. et al. Peripheral T follicular helper Cells Make a Difference in HIV Reservoir Size between Elite Controllers and Patients on Successful cART. Sci Rep 7, 16799 (2017). https://doi.org/10.1038/s41598-017-17057-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-17057-y
This article is cited by
-
Accuracy of real-time PCR and digital PCR for the monitoring of total HIV DNA under prolonged antiretroviral therapy
Scientific Reports (2022)
-
Transcriptional signature of resting-memory CD4 T cells differentiates spontaneous from treatment-induced HIV control
Journal of Molecular Medicine (2020)
-
HIV-2 as a model to identify a functional HIV cure
AIDS Research and Therapy (2019)
-
CD32 Expression is not Associated to HIV-DNA content in CD4 cell subsets of individuals with Different Levels of HIV Control
Scientific Reports (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.