Abstract
Rapid economic development in China has caused marked changes in people’s lifestyles and medical technology. Exploration of stroke subtype trends is necessary to provide physicians with vital insight for early diagnosis and treatment. We included stroke patients admitted from 2006 to 2015. Trends in stroke subtypes and vascular risk factors were investigated. There were 5521 patients, including 4534 (82.1%) ischemic stroke (IS), 813 (14.7%) intracerebral hemorrhage (ICH) and 174 (3.2%) subarachnoid hemorrhage (SAH) patients. The proportion of IS was increasing and proportions of ICH and SAH were decreasing (P < 0.001). Onset age and hypertension remained stable in stroke subtypes. In IS patients, large artery atherosclerosis (LAA) strokes increased from 17.0% to 30.8% in the first 7 years and ultimately decreased to 24.1%. Small vessel disease (SVD) strokes increased from 15.5% to 39.6%, undetermined etiology (UE) strokes decreased from 52.7% to 26.0%, others remained stable. The levels of low-density lipoprotein declined significantly, and an increased number of patients underwent intracranial artery examinations (P < 0.001). In conclusion, proportions of stroke subtypes changed significantly. Anti-hypertension therapy needs to be reinforced to control ICH, SAH and SVD ischemic stroke incidences. The etiologic detection of IS increased and lipid-lowing therapy was effective, cardioembolism detections should be reinforced.
Similar content being viewed by others
Introduction
Strokes are highly prevalent and cause major disabilities worldwide. Both ischemic stroke (IS) and hemorrhage stroke could cause high mortality1. Changes in lifestyle and advances in medical technology during the past decade have likely affected the prevalence of vascular risk factors and thereby the incidence of stroke. It is important for clinicians to have a general impression of the distribution of stroke subtypes to adjust strategies for etiologic detections and to make decisions in diagnosis and therapy2.
IS has been classified into 5 etiologic subtypes, which differ in terms of mechanism, severity, management and prognosis3. Over the past decade, 2 major factors should be considered. First, statins are reported to lower stroke incidence and recurrence through multiple mechanisms4,5. Guidelines for secondary and primary prevention of strokes have recommended the use of statins successively, which would likely lead to enhanced anti-atherosclerosis therapy and a decreased incidence of large artery atherosclerosis (LAA) stroke cases6. Second, the aging of the population might influence some age-related risk factors, such as atrial fibrillation (AF) and, consequently, the number of cardioembolic (CE) stroke cases7.
A few studies have reported IS subtype trends in several other countries2,8,9,10. However, these findings have been inconsistent, and no data from China have been reported. China has different social conditions from other countries and has experienced vast economic development. Therefore, we intended to explore the trends in stroke subtypes, etiology of IS and risk factors in a stroke center in China.
Methods
Study setting and sample
This was a retrospective, hospital-based study. Patients with acute ischemic or hemorrhagic stroke (defined as ≤14 d) admitted to Peking University Third Hospital from January 2006 to December 2015 were included. We excluded patients less than 18 years old and recurrent IS patients in our hospital because the latter cases were likely due to the same IS etiology and may have resulted in an overestimation of the distribution. The patients mainly resided in the Beijing District, the capital city of China. The research was approved by the ethics committee of Peking University Third Hospital. Informed consent was obtained. All methods were performed in accordance with the relevant guidelines and regulations.
The collected data included demographics, stroke risk factors, etiology investigations and ischemic stroke subtypes. Blood pressure was measured on admission. Laboratory investigations were conducted in a fasting state on the second morning after admission. We combined etiologic detection findings by different image technologies to calculate the accomplishment rate in IS patients.
Ischemic subtypes were classified according to the Trial of ORG 10172 in Acute Stroke Treatment (TOAST) criteria11. Briefly, stroke patients were divided into 5 subtypes: LAA, CE, small vessel disease (SVD), other determined etiology (ODE) and undetermined etiology (UE). Specifically, patients with a ≤2 cm size infarct and >50% relevant large artery stenosis on neuroimaging were categorized as having LAA. Ischemic stroke subtypes were evaluated by two independent physicians, and the uncertain cases were discussed to reach a consensus.
Statistical analysis
Quantitative data are presented as the means ± standard deviations (SDs), and qualitative data are presented as numbers and percentages. The data were divided into 3 periods according to admission date: from January 2006 to December 2008, from January 2009 to December 2012, and from January 2013 to December 2015. Analysis of variance (ANOVA) and Chi-squared tests were used for continuous and discrete data separately to analyze the changes in the risk factors among the 3 periods. Binary logistic regression was used to analyze the change in each IS subtype. In each subtype, the proportion in the subsequent year and the average proportions in the earlier years were compared to determine whether significant changes occurred over time. The trends of LAA and SVD strokes were further adjusted for the using vascular investigations. The trend of CE stroke was further adjusted for the using Holter monitoring and echocardiography. All P values are two-sided, and the probability of a type 1 error was set as 0.05. Statistical analyses were performed using SPSS 17.0.
Results
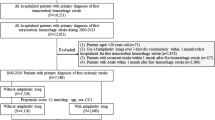
A total of 6483 patients with stroke were admitted to Peking University Third Hospital; 359 patients were excluded because they did not meet the criteria for acute phase stroke, which is less than 14 days after an ischemic stroke. Additionally, 603 patients who visited the same hospital for the second time due to a recurrent stroke were excluded. Therefore, 5521 patients were enrolled in our study. There were 4534 (82.1%) IS patients, 813 (14.7%) intracerebral hemorrhage (ICH) patients and 174 (3.2%) subarachnoid hemorrhage (SAH) patients, 3888 (70.4%) were males. The mean ages were 63.51 ± 13.43 years. In IS patients, there were 3256 (71.8%) males and the mean ages were 64.53 ± 12.82 years. In ICH patients, there were 551 (67.8%) males and the mean ages were 59.33 ± 15.28 years. In SAH patients, there were 81 (46.6%) males and the mean ages were 56.47 ± 13.84 years.
Demographic data and risk factors among the 3 periods are shown in Table 1. Totally, the proportion of IS was increasing and the proportions of ICH and SAH were decreasing (P < 0.001). Onset age did not show a significant change over time (P = 0.337 in IS patients, 0.370 in ICH patients, 0.490 in SAH patients). Male was significantly increasing in IS patients but not in ICH or SAH patients (P = 0.001, 0.695 and 0.596 separately). The mean length of hospital stay continually decreased from 18 days to 14.8 days in IS patients(P < 0.001), and from 19.2 days to 16.4 days in ICH patients (P = 0.014), but did not change significantly in SAH patients (P = 0.302). Regarding the risk factors, the proportion of hypertension remained stable (P = 0.995 in IS patients, 0.927 in ICH patients and 0.453 in SAH patients), and the proportion of diabetes mellitus increased from 29.8% to 40.1% in IS patients (P < 0.001).
When we analyzed IS patients separately, we found that lipid profiles, specifically total cholesterol, triglycerides and low-density lipoprotein decreased continuously during these years (Fig. 1), systolic blood pressure decreased in the former 2 periods and diastolic blood pressure decreased in all 3 periods (Fig. 2). The proportion of AF remained stable (P = 0.812). Additionally, we observed marked increases in the use of intracranial vascular investigations, echocardiography and Holter monitoring (from 25.6% to 75.4%, from 47.4% to 82.6% and from 0.4% to 8.2%, respectively, P < 0.001). The proportion of ischemic stroke subtypes and the association with time are shown in Tables 2 and 3 and Fig. 3.
The incidence of LAA stroke was observed to increase significantly from 17% to 30.8% from 2006 to 2013, and then decrease to 24.1% by 2015. After adjusting for the use of intracranial vascular investigations, no significant increase was observed from 2009 to 2012, and a significant decrease was observed from 2012 to 2015. An increase in SVD strokes was observed, from 15.5% to 39.6%. This trend was still significant after adjusting for the use of intracranial vascular investigations. A significant decrease in UE-related strokes was observed, from 52.7% to 26%. No significant change was observed in the proportion of CE stokes (from 11.0% to 8.4%) in the past decade, even after adjusting for using Holter monitoring and echocardiography. No significant change in ODE strokes was observed.
Discussion
This study showed a temporal trend in stroke subtypes over the past decade, that warrants investigation considering the vast economic development in China. According to World Bank classifications, China has experienced extremely rapid economic growth and has reached a middle income level12. Medical resources have improved, especially in Beijing, the capital of China. Marked changes in industrial and social factors have influenced people’s lifestyle (especially diet composition) and concepts of disabling disease management, such as that for stroke. The aforementioned factors ultimately influence the stroke subtype distribution.
Generally speaking, although the proportion of IS, ICH and SAH patients have changed, they all represented a relatively stable onset age, which is different from a population-based study investigating a low-income district in Tianjin, China, the latter one showed a younger trend of onset age in the past 2 decades13. We suggested one of the reason was that patients in this study were located in a relatively higher income district compared with township in Tianjin, and the stroke prevention worked better. However, the risk factors correlated with specific IS subtypes was changed. The details are as below.
According to previous studies, the proportion of LAA strokes ranges from 14.4% to 57%, which is influenced by ethnicity, region, lifestyle and other factors2,8. In this study, the proportions of the LAA subtype ranged from 17% to 30.8% in different time periods, consistent with other studies in China14. Reportedly, LAA stroke patients have a higher risk of cardiovascular events, stroke recurrence and death15. Atherosclerosis, especially carotid plaque and carotid intima-media thickness, is also closely associated with cardiovascular risk, which is closely associated with risk factors such as blood lipid levels16,17. Statins reportedly aid in the prevention of stroke incidence and recurrence. Since the guidelines for primary stroke prevention recommended statins for anti-atherosclerosis therapy in 2011, statins began to be widely applied6.
The proportion of LAA subtype patients increased in the first 7 years, but decreased in the last 3 years. As we divided the past decade into 3 periods previously, the change was not significant in the 1st and 3rd periods, but was significant in the 2nd period. After adjusting for intracranial vascular investigations, the increasing trend in the 2nd period became non-significant, and the decreasing trend in the 3rd period became significant. Notably, the use of intracranial vascular investigations began to increase in 2009, i.e., the beginning of the 2nd period. Statins were not recommended until 2011, and the 3rd period followed. Therefore, we presumed that the increasing trend in LAA strokes in the 2nd period was due mostly to increasing detection abilities and the availability of stable anti-atherosclerosis therapy. In other words, more LAA stroke subtype patients were diagnosed. In the 3rd period, the etiology detection increased slightly and anti- atherosclerosis therapy was strengthened by using statins, resulting in a significant downtrend of LAA stroke cases. This finding is also consistent with the decreasing lipid profiles and implies that a positive outcome might be achieved by anti-atherosclerosis therapy for the control of LAA strokes.
Hypertension appears to be the most predominant risk factor in the population, contributing to half of the coronary heart disease burden and approximately two-thirds of the cerebrovascular disease burden18. Hypertension is more likely to be correlated with the SVD subtype than the other subtypes in ischemic stroke patients19. Lowering blood pressure could reduce the risk of stroke. Reportedly, when the blood pressure is reduced by 8/4 mmHg, the risk of stroke and other cardiovascular events obviously decreases20. To clarify the underlying reason for the rising trend in the SVD stroke cases, we should first focus on the prevalence and control of hypertension. Based on previous community studies, the hypertension control rate is 9.3% in China compared with 33.1% in America and is also much lower than in several other Asian countries such as Korea, Thailand, and Iran18,21,22. In our study, less efficacy was also shown in hypertension control. The number of patients with hypertension remained stable over the past decade, and the decrease in blood pressure was slight. Briefly, anti-hypertensive therapy should be reinforced to control the incidence of SVD stroke cases.
Unlike those in other countries, CE stroke cases did not increase in our study. The proportion fluctuated between 11% and 8.4%, much lower than the values reported in other studies such as the German stroke data bank (25% CE strokes)23,24. Once CE sources are recognized, anti-coagulation treatment should start. Early diagnosis is very important.
AF is the most common cause in CE stroke cases. In this study, stroke with AF accounted for approximately 7% to 8% of all ischemic stroke types, similar to values reported in Canada (8–11%) but much lower than values reported in Poland (24.6–31.7%). There are several risk factors for AF, such as hypertension, coronary heart disease and age25,26. A high proportion of coronary heart disease and the increasing onset age may contribute to the high AF rate in Poland. The onset age in our study did not increase, possibly partially due to the less effective measures for risk factors, since successful control measures for hypertension, diabetes mellitus and dyslipidemia are suspected to delay the onset age of strokes. Additionally, we also need to consider the detection rate. Paroxysmal AF becomes more detectable as the electrocardiographic (ECG) monitoring period is prolonged27. Holter monitoring is recommended to improve AF detection. In our study, all patients underwent 12-lead ECG monitoring on admission, but the proportion of patients who underwent 24-h Holter monitoring was only 0.4–8.2%, which was much lower than in reports from Canada (13–46%) and Poland (26–62.5%)2,8. It is easy to conclude that AF detection in China is less valued and needs to be reinforced among UE stroke patients.
The time trends in stroke subtypes in this study were much different from those of other countries. Here, we summarized previous studies in Canada, Korea, Poland and Japan2,8,10,22. An increasing trend was observed in CE strokes, and a decreasing trend was observed in SVD strokes in Canada, Korea, and Poland. However, LAA strokes declined in Canada, remained stable in Korea, and showed an increasing trend in Poland. A community-based study in Japan showed an increasing trend in CE strokes, with a decreased trend in non-lacunar strokes. Consistently, the UE stroke subtype remained stable in previous studies. In China, LAA stroke showed a single apex trend, CE stroke was low and stable, SVD stroke kept increasing and UE stroke kept decreasing, findings that are much different from those from other countries.
We also investigated the trend of ICH and SAH in the past decade. We found that there is a relatively stable proportion of hypertension, which suggests us the hypertension management should also be improved in the prevention of hemorrhagic stroke.
Our study has several advantages. Although several studies have investigated the stroke subtype trends, the situation in China remains unknown. China has different ethnic and lifestyle conventions than Western European and North American countries, and its economic status is different from other reported Asian countries, such as Korea and Japan. Considering the severe disease burden in China28, further investigations of the stroke subtype distribution and trends are necessary. Our study had a large sample size, which included patients admitted to our stroke center over 10 years. The electronic medical records in the hospital were accurate, and the evaluation of the TOAST subtype by neurological physicians was relatively precise.
However, this study has several limitations. First, this is a retrospective study, and some data, such as the national institutes of health stroke scale (NIHSS) score, were not available for all patients. Therefore, we cannot compare the stroke severity in different years, which may influence the proportion of stroke subtypes. Second, this is a hospital-based study. Therefore, the interpretation of the etiology should be restricted to this center, although the changes in etiology may be influenced by patients’ tendency to seek medical care and changes in the natural population. However, based on these data, the number of admitted stroke patients each year and the average age of the patients did not substantially change, suggesting a relatively steady patient source. Third, this is a single-center study and may not be fully representative of all Chinese patients. Therefore, multi-center and population-based studies are needed to determine the changes in stroke subtypes and stroke risk factors over time.
References
Thrift, A. G. et al. Global stroke statistics: An update of mortality data from countries using a broad code of “cerebrovascular diseases”. International journal of stroke: official journal of the International Stroke Society 12, 796–801, https://doi.org/10.1177/1747493017730782 (2017).
Bogiatzi, C., Hackam, D. G., McLeod, A. I. & Spence, J. D. Secular trends in ischemic stroke subtypes and stroke risk factors. Stroke 45, 3208–3213, https://doi.org/10.1161/strokeaha.114.006536 (2014).
Hao, Z. et al. Etiologic subtype predicts outcome in mild stroke: prospective data from a hospital stroke registry. BMC neurology 13, 154, https://doi.org/10.1186/1471-2377-13-154 (2013).
Amarenco, P. et al. High-dose atorvastatin after stroke or transient ischemic attack. The New England journal of medicine 355, 549–559, https://doi.org/10.1056/NEJMoa061894 (2006).
Cimino, M. et al. Statins: multiple mechanisms of action in the ischemic brain. The Neuroscientist: a review journal bringing neurobiology, neurology and psychiatry 13, 208–213, https://doi.org/10.1177/1073858406297121 (2007).
Goldstein, L. B. et al. Guidelines for the primary prevention of stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 42, 517–584, https://doi.org/10.1161/STR.0b013e3181fcb238 (2011).
Long, X. et al. Mortality, Recurrence, and Dependency Rates Are Higher after Acute Ischemic Stroke in Elderly Patients with Diabetes Compared to Younger Patients. Frontiers in aging neuroscience 8, 142, https://doi.org/10.3389/fnagi.2016.00142 (2016).
Bembenek, J. P. et al. Temporal trends in vascular risk factors and etiology of urban Polish stroke patients from 1995 to 2013. Journal of the neurological sciences 357, 126–130, https://doi.org/10.1016/j.jns.2015.07.011 (2015).
Jung, K. H. et al. Secular trends in ischemic stroke characteristics in a rapidly developed country: results from the Korean Stroke Registry Study (secular trends in Korean stroke). Circulation. Cardiovascular quality and outcomes 5, 327–334, https://doi.org/10.1161/circoutcomes.111.963736 (2012).
Turin, T. C. et al. Ischemic stroke subtypes in a Japanese population: Takashima Stroke Registry, 1988-2004. Stroke 41, 1871–1876, https://doi.org/10.1161/strokeaha.110.581033 (2010).
Adams, H. P. et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24, 35–41 (1993).
The World Bank, http://data.worldbank.org/country (2017).
Wang, J. et al. Trends in Age of First-Ever Stroke Following Increased Incidence and Life Expectancy in a Low-Income Chinese Population. Stroke 47, 929–935, https://doi.org/10.1161/strokeaha.115.012466 (2016).
Tsai, C. F., Thomas, B. & Sudlow, C. L. Epidemiology of stroke and its subtypes in Chinese vs white populations: a systematic review. Neurology 81, 264–272, https://doi.org/10.1212/WNL.0b013e31829bfde3 (2013).
Amarenco, P. et al. One-Year Risk of Stroke after Transient Ischemic Attack or Minor Stroke. The New England journal of medicine 374, 1533–1542, https://doi.org/10.1056/NEJMoa1412981 (2016).
Naqvi, T. Z. & Lee, M. S. Carotid intima-media thickness and plaque in cardiovascular risk assessment. JACC. Cardiovascular imaging 7, 1025–1038, https://doi.org/10.1016/j.jcmg.2013.11.014 (2014).
Chen, P. C. et al. Carotid Atherosclerosis Progression and Risk of Cardiovascular Events in a Community in Taiwan. Scientific reports 6, 25733, https://doi.org/10.1038/srep25733 (2016).
Wang, J., Zhang, L., Wang, F., Liu, L. & Wang, H. Prevalence, awareness, treatment, and control of hypertension in China: results from a national survey. American journal of hypertension 27, 1355–1361, https://doi.org/10.1093/ajh/hpu053 (2014).
Lv, P. et al. Comparison of Risk Factor between Lacunar Stroke and Large Artery Atherosclerosis Stroke: A Cross-Sectional Study in China. PloS one 11, e0149605, https://doi.org/10.1371/journal.pone.0149605 (2016).
Turnbull, F. Effects of different blood-pressure-lowering regimens on major cardiovascular events: results of prospectively-designed overviews of randomised trials. Lancet (London, England) 362, 1527–1535 (2003).
Ong, K. L., Cheung, B. M., Man, Y. B., Lau, C. P. & Lam, K. S. Prevalence, awareness, treatment, and control of hypertension among United States adults 1999-2004. Hypertension 49, 69–75, https://doi.org/10.1161/01.hyp.0000252676.46043.18 (2007).
Lee, H. S. et al. Prevalence, awareness, treatment and control of hypertension in adults with diagnosed diabetes: the Fourth Korea National Health and Nutrition Examination Survey (KNHANES IV). Journal of human hypertension 27, 381–387, https://doi.org/10.1038/jhh.2012.56 (2013).
Grau, A. J. et al. Risk factors, outcome, and treatment in subtypes of ischemic stroke: the German stroke data bank. Stroke 32, 2559–2566 (2001).
Pistoia, F. et al. The Epidemiology of Atrial Fibrillation and Stroke. Cardiology clinics 34, 255–268, https://doi.org/10.1016/j.ccl.2015.12.002 (2016).
Thijs, V. & Butcher, K. Challenges and misconceptions in the aetiology and management of atrial fibrillation-related strokes. European journal of internal medicine 26, 461–467, https://doi.org/10.1016/j.ejim.2015.06.008 (2015).
Andersson, P., Londahl, M., Abdon, N. J. & Terent, A. The prevalence of atrial fibrillation in a geographically well-defined population in northern Sweden: implications for anticoagulation prophylaxis. Journal of internal medicine 272, 170–176, https://doi.org/10.1111/j.1365-2796.2012.02519.x (2012).
Choe, W. C. et al. A Comparison of Atrial Fibrillation Monitoring Strategies After Cryptogenic Stroke (from the Cryptogenic Stroke and Underlying AF Trial). The American journal of cardiology 116, 889–893, https://doi.org/10.1016/j.amjcard.2015.06.012 (2015).
Liu, L., Wang, D., Wong, K. S. & Wang, Y. Stroke and stroke care in China: huge burden, significant workload, and a national priority. Stroke 42, 3651–3654, https://doi.org/10.1161/strokeaha.111.635755 (2011).
Acknowledgements
This study was supported by grants from the National Natural Sciences Foundation of China (81471184) and the Capital Health Research and Development of Special (No. 2014-1-4092).
Author information
Authors and Affiliations
Contributions
Danyang Tian and Qiong Yang designed the detailed protocol and analyzed the result, Danyang Tian and Quan Dong separately evaluated the TOAST subtypes and Nan Li gave suggestions on statistical methods. Dongsheng Fan conceived the research and guided the process. Danyang Tian, Qiong Yang, Bernard Yan and Dongsheng Fan wrote the main manuscript and prepared the tables and figures. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tian, D., Yang, Q., Dong, Q. et al. Trends in stroke subtypes and vascular risk factors in a stroke center in China over 10 years. Sci Rep 8, 5037 (2018). https://doi.org/10.1038/s41598-018-23356-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-23356-9
This article is cited by
-
A Mendelian randomization analysis of the relationship between cardioembolic risk factors and ischemic stroke
Scientific Reports (2021)
-
Recanalization Treatment for Acute Stroke: Can We Skip the Bridge?
Neuroscience Bulletin (2021)
-
In-hospital recurrence in a Chinese large cohort with acute ischemic stroke
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.