Abstract
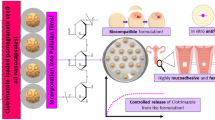
The development of vaginal medications, especially antifungal medications, requires that the drug is solubilized as well as retained at or near the mucosa for sufficient periods of time to ensure adequate bioavailability. Itraconazole is a broad-spectrum antifungal agent, which has been used for some time orally and intravenously but for which a vaginal formulation has not yet been developed. We present here a novel itraconazole formulation intended for vaginal use based on hydroxypropyl-β-cyclodextrin (HPβCD), a functional excipient that increases drug solubility and generates a mucoadhesive system in the presence of other ingredients. An aqueous phase was prepared by solubilizing itraconazole with HCl in the presence of propylene glycol and then adding an aqueous solution of HPβCD. After pH adjustment, the itraconazole/HPβCD solution was added to the oil phase (paraffin oil, trihydroxystearate, and cetyl dimethicon copolyol) and the desired cream containing 1%, 2%, and 2.5% drug obtained by homogenization. Primary irritation studies and subchronic toxicity studies using a rabbit vaginal model indicated that the formulation was safe, well tolerated, and retained in the vaginal space. Clinical investigations indicated that application of 5 g of a 2% cream was very well tolerated and itraconazole was not systemically absorbed. Additional studies in women found that the itraconazole cream was highly effective in reducing or eliminating fungal cultures with few adverse effects. These studies suggested that an HPβCD-based, emulsified wax cream formulation was a useful and effective dosage form for treating vaginal candidiasis.
Similar content being viewed by others
References
Grant S, Clissold S. Itraconazole: a review of its pharmacodynamic and pharmacokinetic properties and therapeutic use in superficial and systemic mycoses. Drugs. 1989; 37: 310–344.
De Beule K, Van Gestel J. Pharmacology of itraconazole. Drugs. 2001; 61(suppl 1): 27–33.
Jain S, Sehgal V. Itraconazole: an effective oral antifungal for onchyomychosis. Int J Dermatol. 2001; 40: 1–5.
Bloch G, Barnard PG, Burger GD, Meyer JS, Parkes JR, Smythe E. Itraconazole in the treatment of acute vaginal candidiasis. S Afr Med J. 1988; 73: 172–173.
Sanz F, Del Palacio Hermanz A. Randomized comparative trial of three regimens of itraconazole for treatment of vaginal mycoses. Rev Infect Dis. 1987; 9(suppl 1): S139-S142.
Larosa E, Cauwenbergh G, Cilli P, Woestenborghs R, Heykants J. Itraconazole pharmacokinetics in the female genital tract: plasma and tissue levels in patients undergoing hysterectomy after a single dose of 200 mg itraconazole. Eur J Obstet Gynecol. 1986; 23: 85–89.
Ross RA, Lee MT, Onderdonk AB. Effect of Candida albicans infection and clotrimazole treatment on vaginal microflora in vitro. Obstet Gynaecol. 1995; 86: 925–930.
Chang JY, Oh Y-K, Kong HS, Kim EJ, Jang DD, Nam KT, Kim C-K. Prolonged antifungal effects of clotrimazole-containing mucoadhesive thermosensitive gels on vaginitis. J Control Rel. 2002; 82: 39–50.
Chang JY, Oh Y-K, Choi H-G, Kim YB, Kim C-K. Rheological evaluation of thermosensitive and mucoadhesive vaginal gels in physiological conditions. Int J Pharm. 2002; 241: 155–163.
Putteman P, Francois M, Snoeckx E, inventors, Janssen Pharmaceutica Mucoadhesive emulsions containing cyclodextrins. US Patent 5814220/WO9531178. November 23, 1995.
Vermani K, Garg S, Zaneveld L. Assemblies for in vitro measurement of bioadhesive strength and retention characteristics in simulated vaginal environment. Drug Dev Ind Pharm. 2002; 28: 1133–1146.
Woodley J. Bioadhesion: new possibilities for drug administration? Clin Pharmacokinet. 2001; 40: 77–84.
Peeters J, Neeskens P, Tollenaere JP, Van Remoortere P, Brewster ME. Characterization of the interaction of 2-hydroxypropyl-β-cyclodextrin with itraconazole at pH 2, 4 and 7. J Pharm Sci. 2002; 91: 1414–1422.
Miyake K, Irie T, Arima H, Hirayama F, Uekama K, Hirano M, Okamoto Y. Characterization of itraconazole/2-hydroxypropyl-β-cyclodextrin inclusion complex in aqueous propylene glycol solution. Int J Pharm. 1999; 179: 237–245.
Loftsson T, Brewster M. Pharmaceutical applications of cyclodextrins. I. Drug solubilization and stabilization. J Pharm Sci. 1996; 85: 1017–1025.
Michaud M, Icart S. Determination of the substitution of hydroxypropylbetadex using Fourier transform infrared spectrophotometry. PharmEuropa. 2001; 13: 714–716.
Higuchi T, Connors K. Phase-solubility techniques. Adv Anal Chem Instrum. 1965; 4: 117–212.
Woestenborghs R, Lorreyne W, Heykants J. Determination of itraconazole in plasma and animal tissues by high-performance liquid chromatography. J Chromatogr. 1987; 413: 332–337.
Heykants J, Van Peer A, Van de Velde V, Van Rooy P, Meuldermans W, Lavrijsen K, Woestenborghs R, Van Custem J, Cauwenbergh G. The clinical pharmacokinetics of itraconazole: an overview. Mycoses. 1989; 32(suppl 1): 67–87.
Upmalis D, Lamia C, Harley J, Cone F. A new formulation of miconazole nitrate in the treatment of vulvovaginal candidiasis. Adv Therap. 1998; 15: 14–22.
Author information
Authors and Affiliations
Corresponding author
Additional information
Published: March 6, 2003
Rights and permissions
About this article
Cite this article
Francois, M., Snoeckx, E., Putteman, P. et al. A mucoadhesive, cyclodextrin-based vaginal cream formulation of itraconazole. AAPS PharmSci 5, 5 (2003). https://doi.org/10.1208/ps050105
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/ps050105