Abstract
Background
The tumor-node-metastasis classification system has proposed that lung cancers presenting as multifocal ground-glass nodules (multi-GGN) on computed tomography scan should be staged as multiple primaries instead of intrapulmonary metastases. However, the problem still exists for those synchronous multiple lung adenocarcinomas (SMLA) involving solid lesions. This study aimed to explore the distinct features of SMLA to better define the diagnosis and staging of this disease.
Methods
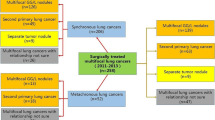
Between 2008 and 2016, consecutive patients with complete resection of SMLA were prospectively enrolled in the study. The patients were divided into three groups based on CT images as follows: multi-GGN, one solid nodule plus one or more GGNs (solid-GGN), and multiple solid lesions with or without GGN (multi-solid). Clinicopathologic features and survival outcomes were compared between these groups. Multivariate Cox proportional hazards analyses using bootstrap internal validation were performed to identify independent predictors for recurrence-free survival (RFS) and overall survival (OS).
Results
Of the 695 patients who met the inclusion criteria, 486 (69.9%) presented with multi-GGN tumor, 124 (17.9%) with solid-GGN tumor, and 85 (12.2%) with multi-solid tumor. The three groups had distinguished clinicopathologic features of gender, smoking history, nodal metastases, tumor size, subtype, and location (all P < 0.001). Multivariate analyses demonstrated that multi-solid tumor was an independent predictor for both decreased RFS [hazard ratio (HR) 2.941; 95% confidence interval (CI) 1.07–8.08; P = 0.036] and poor OS (HR 6.13; 95% CI 1.15–32.63; P = 0.034), but neither RFS (P = 0.384) nor OS (P = 0.811) differed between solid-GGN and multi-GGN tumors.
Conclusions
Both multi-GGN and solid-GGN tumors should be staged as multiple primaries, whereas multi-solid tumor was indicated to be advanced disease.



Similar content being viewed by others
References
Ishikawa Y, Nakayama H, Ito H, et al. Surgical treatment for synchronous primary lung adenocarcinomas. Ann Thorac Surg. 2014;98:1983–8.
Zhang Y, Hu H, Wang R, et al. Synchronous non-small cell lung cancers: diagnostic yield can be improved by histologic and genetic methods. Ann Surg Oncol. 2014;21:4369–74.
Martini N, Melamed MR. Multiple primary lung cancers. J Thorac Cardiovasc Surg. 1975;70:606–12.
Chung JH, Choe G, Jheon S, et al. Epidermal growth factor receptor mutation and pathologic-radiologic correlation between multiple lung nodules with ground-glass opacity differentiates multicentric origin from intrapulmonary spread. J Thorac Oncol. 2009;4:1490–5.
Girard N, Deshpande C, Lau C, et al. Comprehensive histologic assessment helps to differentiate multiple lung primary non-small cell carcinomas from metastases. Am J Surg Pathol. 2009;33:1752–64.
Girard N, Deshpande C, Azzoli CG, et al. Use of epidermal growth factor receptor/Kirsten rat sarcoma 2 viral oncogene homolog mutation testing to define clonal relationships among multiple lung adenocarcinomas: comparison with clinical guidelines. Chest. 2010;137:46–52.
Warth A, Macher-Goeppinger S, Muley T, et al. Clonality of multifocal non-small cell lung cancer: implications for staging and therapy. Eur Respir J. 2012;39:1437–42.
Murphy SJ, Aubry MC, Harris FR, et al. Identification of independent primary tumors and intrapulmonary metastases using DNA rearrangements in non-small cell lung cancer. J Clin Oncol. 2014;32(36):4050–8.
Sun W, Liu Y, Liu XY, Lin DM, Lv N. Significance of nonmucinous lepidic component with mild nuclear atypia in the discrimination of multiple primary lung cancers from intrapulmonary metastases. Int J Clin Exper Pathol. 2014;7:7583–96.
Detterbeck FC, Nicholson AG, Franklin WA, et al. The IASLC Lung Cancer Staging Project: summary of proposals for revisions of the classification of lung cancers with multiple pulmonary sites of involvement in the forthcoming eighth edition of the TNM classification. J Thorac Oncol. 2016;11:639–50.
Gu B, Burt BM, Merritt RE, et al. A dominant adenocarcinoma with multifocal ground glass lesions does not behave as advanced disease. Ann Thorac Surg. 2013;96:411–8.
Ye T, Deng L, Wang S, et al. Lung adenocarcinomas manifesting as radiological part-solid nodules define a special clinical subtype. J Thorac Oncol. 2019;14:617–27.
Fu F, Zhang Y, Wen Z, et al. Distinct prognostic factors in patients with stage I non-small cell lung cancer with radiologic part solid or solid lesions. J Thorac Oncol. 2019;14(12):2133–42.
Ye T, Deng L, Xiang J, et al. Predictors of pathologic tumor invasion and prognosis for ground-glass opacity featured lung adenocarcinoma. Ann Thorac Surg. 2018;106:1682–90.
Liu S, Wang R, Zhang Y, et al. Precise diagnosis of intraoperative frozen section is an effective method to guide resection strategy for peripheral small-sized lung adenocarcinoma. J Clin Oncol. 2016;34:307–13.
Ettinger DS, Wood DE, Akerley W, et al. Non-small cell lung cancer, version 1.2015. JNCCN J Natl Comprehensive Cancer Network. 2014;12:1738–61.
Travis WD, Brambilla E, Noguchi M, et al. International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society International Multidisciplinary Classification of Lung Adenocarcinoma. J Thorac Oncol. 2011;6:244–85.
Warth A, Muley T, Meister M, et al. The novel histologic International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society classification system of lung adenocarcinoma is a stage-independent predictor of survival. J Clin Oncol. 2012;30:1438–46.
Hu H, Sun Z, Li Y, et al. The histologic classifications of lung adenocarcinomas are discriminable by unique lineage backgrounds. J Thorac Oncol. 2016;11(12):2161–72.
Zhang Y, Wang R, Cai D, et al. A comprehensive investigation of molecular features and prognosis of lung adenocarcinoma with micropapillary component. J Thorac Oncol. 2014;9:1772–8.
Zhang Y, Li J, Wang R, et al. The prognostic and predictive value of solid subtype in invasive lung adenocarcinoma. Sci Rep. 2014;4:7163.
Tsao MS, Marguet S, Le Teuff G, et al. Subtype classification of lung adenocarcinoma predicts benefit from adjuvant chemotherapy in patients undergoing complete resection. J Clin Oncol. 2015;33:3439–46.
Gazdar AF, Minna JD. Multifocal lung cancers: clonality vs field cancerization and does it matter? J Natl Cancer Institute. 2009;101:541–3.
Detterbeck FC, Marom EM, Arenberg DA, et al. The IASLC Lung Cancer Staging Project: background data and proposals for the application of TNM staging rules to lung cancer presenting as multiple nodules with ground-glass or lepidic features or a pneumonic type of involvement in the forthcoming eighth edition of the TNM classification. J Thorac Oncol. 2016;11:666–80.
Detterbeck FC, Franklin WA, Nicholson AG, et al. The IASLC Lung Cancer Staging Project: background data and proposed criteria to distinguish separate primary lung cancers from metastatic foci in patients with two lung tumors in the forthcoming eighth edition of the TNM classification for lung cancer. J Thorac Oncol. 2016;11:651–65.
Detterbeck FC, Bolejack V, Arenberg DA, et al. The IASLC Lung Cancer Staging Project: background data and proposals for the classification of lung cancer with separate tumor nodules in the forthcoming eighth edition of the TNM classification for lung cancer. J Thorac Oncol. 2016;11:681–92.
Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT. The 8th-edition lung cancer stage classification. Chest. 2017;151(1):193–203.
Kadota K, Nitadori J, Sima CS, et al. Tumor spread through air spaces is an important pattern of invasion and impacts the frequency and location of recurrences after limited resection for small stage I lung adenocarcinomas. J Thorac Oncol. 2015;10:806–14.
Kim HK, Choi YS, Kim K, et al. Management of ground-glass opacity lesions detected in patients with otherwise operable non-small cell lung cancer. J Thorac Oncol. 2009;4:1242–6.
Donington JS. An additional step toward personalization of surgical care for early-stage non-small cell lung cancer. J Clin Oncol. 2016;34:295–6.
Baisi A, De Simone M, Raveglia F, Cioffi U. What really affects synchronous pulmonary adenocarcinoma management? Ann Thorac Surg. 2015;100:1506–7.
Zhao Y, Wang R, Shen X, et al. Minor components of micropapillary and solid subtypes in lung adenocarcinoma are predictors of lymph node metastasis and poor prognosis. Ann Surg Oncol. 2016;23:2099–105.
Acknowledgments
This work was supported by grants from The National Natural Science Foundation of China (81572253), the Shanghai Shenkang Hospital Development Center City Hospital Emerging Cutting-Edge Technology Joint Research Project (SHDC12017102), and the Shanghai Municipal Health Commission Key Discipline Project (2017ZZ02025 and 2017ZZ01019).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosure
The author declares that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, Y., Li, G., Li, Y. et al. Imaging Features Suggestive of Multiple Primary Lung Adenocarcinomas. Ann Surg Oncol 27, 2061–2070 (2020). https://doi.org/10.1245/s10434-019-08109-w
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-019-08109-w